CPD: Improving detection and management of atrial fibrillation
Advanced nurse practitioner Beverley Bostock explains the criteria for identifying and diagnosing non-valvular atrial fibrillation and provides a rationale for the treatment and ongoing management of the condition in this CPD module.
The diagnosis and management of atrial fibrillation (AF) has been identified as a key priority for the NHS, primarily because of the link between AF and stroke. In 2019 Public Health England set a 10-year target of improving cardiovascular outcomes through better detection and treatment of AF, hypertension, dyslipidaemia and heart failure.1 Over one million people in the UK have been diagnosed with AF but up to half a million more remain undiagnosed.2 The European Society of Cardiology estimates that one in three of the population will develop AF in their lifetime.3 AF symptoms can impact on people’s quality of life, but it is the risk of AF-related stroke which drives the need to detect the condition, protect people from clot formation which can lead to strokes and perfect the approach to anticoagulation, based on the needs and preferences of the individual.
Related Article: Diagnosis Connect service will link people to advice from charities
AF is an arrhythmia which occurs because of misfiring electrical impulses from the pulmonary vein interacting with abnormal atrial tissue. As a result of this disordered activity, small clots can form in the atria, which can travel to the brain causing a stroke.4 AF-related strokes are more devastating than non-AF related strokes in terms of their morbidity and mortality.5 Although some people with AF will have symptoms such as palpitations, breathlessness, chest pain or fatigue, up to 40% of people with AF have no symptoms.6 This means that healthcare professionals (HCPs) should proactively seek out undiagnosed AF by performing and teaching pulse checks. If people are taught to check their own pulse, they can do this regularly, increasing the chance of picking up an irregular pulse which might indicate an asymptomatic arrhythmia. Arrhythmia Alliance has some useful resources to support HCPs who want to teach people to do this (see resources section for details).
The full module will guide you through:
- Why it is important to recognise and diagnose atrial fibrillation (AF)
- The risk factors for AF – which groups should be targeted for assessment
- Making the diagnosis – history, examination and objective tests
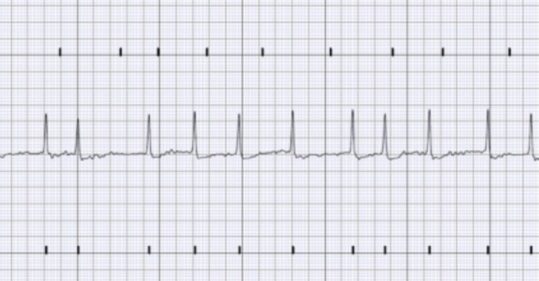
- Interpreting the electrocardiogram (ECG)
- Initiating treatment – the role of direct oral anticoagulants (DOACs) and warfarin
- The principles of ongoing management
Author
Beverley Bostock is an Advanced Nurse Practitioner, PCN Nurse co-ordinator in Hereford and Primary Care Cardiovascular Society Council Member.
Related Article: CVD prevention must be national health priority, says report
Find this module
The full CPD module can be found on the Nursing in Practice 365 website.
Related Article: Prescribing in England to be led by a single national formulary
Not a Nursing in Practice 365 subscriber? Register for free or gain access to more CPD content as a Premium member.

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom




