Choosing the right emollients for eczema
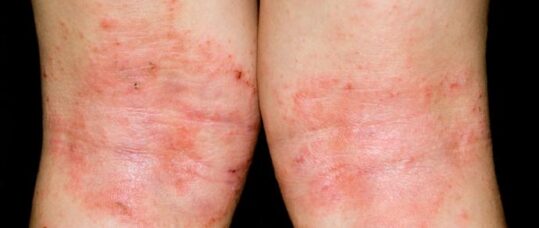
Emollients are commonly prescribed for dry skin conditions such as eczema and should be used alongside anti-inflammatory treatments such as topical corticosteroids.
There are three methods of application of emollients:1
- Leave-on (directly applied) emollients, where emollients are applied to the skin and left to soak in.
- Soap substitutes, where emollients are used instead of soap or other washing products.
- Bath emollients (or bath additives).
Emollients are available in a variety of formulations: creams, ointments, gels, lotions, sprays, washes, and bath and shower additives.
Products can be further classified as simple emollients with no additional ingredients or they may have active ingredients, which may be indicated for some people (see Box 1).
Related Article: Diagnosis Connect service will link people to advice from charities
Simple emollients put a fine moisture-retaining layer of non-physiologic lipid or oil, such as petrolatum or mineral oil, over the skin surface and thereby reduce water loss from the stratum corneum.
More advanced emollient products contain additional ingredients, including humectants such as urea and glycerol, which attract and hold water in the stratum corneum.2
| Box 1 Active ingredients in emollients2,3 |
|---|
|
Prescribing emollients should not be based purely on cost alone, there are several factors to consider prior to this (see Box 2) and there is no evidence from controlled trials to support the use of one emollient over another. The following unanswered questions relating to emollient use and eczema have been highlighted by research and require further investigation:3,4,5
- Which emollient is the most effective and safe in treating eczema?
- What determines patient choice and use of emollients and does choice affect outcome?
- What is the optimal amount of emollient to use?
- What are the most harmful and beneficial ingredients of an emollient?
| Box 2 Factors to consider when prescribing emollients3,6 |
|---|
|
Emollient choice and product use should be based both on the clinical assessment and patient preference. Many of the products available can be used for washing, bathing, showering and moisturising. Bath emollients are widely prescribed for childhood eczema, yet evidence of their benefits over direct application of emollients is lacking and a study is currently underway.1
Prescribing of emollients should include providing adequate quantities (500g per week) as they are typically under-prescribed and under-used, which results in suboptimal treatment of dry skin and eczema, and may increase the occurrence of flares.3 Prescribing should also include further advice regarding the correct and safe use of emollients.7,8
Prescribing emollients in pumps or tubes reduces this risk. Following a skin infection, new supplies of the emollient should be prescribed.
Related Article: CVD prevention must be national health priority, says report
Using emollients on a regular basis either at home, or in a caring environment such as a care home, can increase the risk of slippage because there will be a build-up of grease on the floor and bathroom facilities unless measures are taken.
The floor should be protected with a towel or bath mat and the bath/shower should be washed with hot water and washing-up liquid (detergent) after use, rinsed well and dried with paper towels. This prevents a build-up of emollient and skin debris on the surface and reduces the risk of infection and slipping. It also helps to clear the drains. I have had several patients tell me that their drains were blocked resulting from a build-up of grease and skin debris.
Recently there has been a further alert from the Medicines and Healthcare Products Regulatory Agency (MHRA) relating the fire risk associated with paraffin-based emollients (such as white soft paraffin, white soft paraffin 50%/liquid paraffin 50% or emulsifying ointment) on dressings or clothing and the use of aqueous cream, which may cause burning, stinging, itching and redness, especially in children with atopic eczema.3
Aqueous cream contains sodium lauryl sulphate, which has a detrimental effect on skin barrier function and dermatology specialists do not recommend its use either as a wash or leave-on product, there are other emollient formulations, which are better and which have a positive effect on skin barrier function.
Sandra Lawton is nurse consultant dermatology for Rotherham NHS Foundation Trust
Related Article: Postnatal contraception advice reduces the risk of back-to-back pregnancies
References
- Santer M, Rumsby K, Ridd MJ, et al. Bath additives for the treatment of childhood eczema (BATHE): protocol for multicentre parallel group randomised trial. BMJ Open 2015;5:e009575
- Moncrieff G, Cork M, Lawton S, et al. Use of emollients in dry-skin conditions: consensus statement. Clin Exp Dermatol 2013;38:231-8
- NICE. CKS: Eczema – atopic. London;NICE:2017
- Van Zuuren EJ, Fedorowicz Z, Arents BWM. Emollients and moisturizers for eczema: abridged Cochrane systematic review including GRADE assessments. Br J Dermatol 2017;177:1256-71
- Batchelor JM, Ridd MJ, Clarke T, et al. The Eczema Priority Setting Partnership: A collaboration between patients, carers, clinicians and researchers to identify and prioritise important research questions for the treatment of eczema. Br J Dermatol;168:577-82
- Oakley R, Lawton S. Views on unwanted effects of leave-on emollients and experiences surrounding their incidence. Dermatol Nurs 2016;15:38-43
- National Eczema Society. Emollients. London;NES:2016
- Lawton S. ‘No one told me that’ – using topical treatments safely. London;Nursing in Practice:2017
Nursing in Practice Events visit 12 locations across the UK and cover topics such as dermatology. If you would like to learn more please visit nursinginpractice-events.co.uk

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom


Emollients are commonly prescribed for dry skin conditions such as eczema and should be used alongside anti-inflammatory treatments such as topical corticosteroids.



