CPD: Case by case – managing common skin infections in primary care
Dermatology nurse specialist Julie Van Onselen explains the appropriate diagnosis and management of common skin infections through a series of six hypothetical case studies
Module summary
Skin conditions are the commonest presentations in general practice, making up 24% of consultations.1 The most frequent diagnostic group is skin infections, with the top three infections being cellulitis, fungal infections and impetigo. This module will use a series of six illustrative cases to discuss evidence-based management of some common skin infections in primary care. The treatment advice is based on current NICE, British Association of Dermatology (BAD) and Primary Care Dermatology Society (PCDS) guidance.
Learning objectives
Related Article: Diagnosis Connect service will link people to advice from charities
- Improve understanding of common skin infections in primary care
- Recognise key history and features associated with these infections
- Enhance knowledge of available treatment options for common skin infections
- Understand the appropriate public health considerations, and gain confidence with advising and supporting patients in the management of skin infections
- Know the red flags with common skin infections
All cases are hypothetical and do not involve real patients; they were developed for illustrative purposes only
Case study 1. Toddler with crusty facial lesions
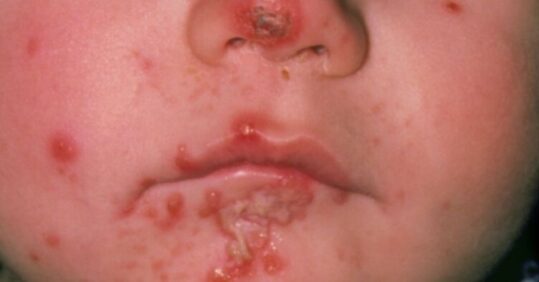
An 18-month child, who is at nursey school, develops clusters of yellow crusty lesions on her face around the nose and mouth. Over the next week, while waiting for an appointment at the GP surgery, the lesions start to blister and weep (see image). Other children start to show similar symptoms, without blistering.
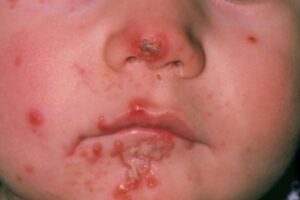
Image: Crusty lesions on face of infant
- What condition does this infant, and the other children with similar symptoms have?
This case is an example of an outbreak of impetigo in a nursery school. Impetigo is a common skin infection, usually caused by Staphylococcus aureus bacteria, which is highly contagious.
The presence of blisters (bullae) is called bullous impetigo and indicates more severe infection. Another key difference between the bullous and non-bullous forms is that buccal mucous membrane can be involved in bullous impetigo. 2 Oral antibiotics are required to treat bullous impetigo, whereas non-bullous impetigo can generally be treated with topical therapies.
- What is the treatment and public health advice?
First-line treatment of localised, non-bullous impetigo is topical antiseptic hydrogen peroxide 1% cream, which should be applied 2-3 times a day for 5 days. Topical antibiotics are now only recommended as second-line treatments (or if 1% hydrogen peroxide is unsuitable).3
Related Article: CVD prevention must be national health priority, says report
In this case, the infant has more extensive infection and blisters, indicating bullous impetigo, so in addition to topical 1% hydrogen peroxide, will require oral antibiotics straight away. The recommended first-line antibiotic is flucloxacillin, for 5 days (if unsuitable, clarithromycin 25mg). Oral and topical antibiotics should not be used concurrently.3
It is important to advise parents on good hygiene measures, including hand-washing and not to share towels, to help reduce the spread of infection. The BAD website provides a useful patient information leaflet. Children should be kept off nursery or school until lesions have crusted and healed, or until 48 hours after antibiotic treatment was started.
If impetigo does not clear with treatment, or becomes worse, the differential diagnosis may include erysipelas, or staphylococcal scaling skin syndrome. NICE recommends a skin swab for microbiological testing to guide diagnosis and treatment.3
Note that in England community pharmacists can now treat non-bullous impetigo through the Pharmacy First initiative – patients can be signposted to this service, which in this case may have helped the child get treatment earlier for the infection and potentially avoid antibiotics.
To complete the full module visit the Nursing in Practice 365 website.
Related Article: Postnatal contraception advice reduces the risk of back-to-back pregnancies
Not a Nursing in Practice 365 subscriber? Register for free or gain access to more CPD content as a Premium member.
Julie Van Onselen is a Dermatology Lecturer Practitioner at Dermatology Education Partnership Ltd and clinical advisor for the National Eczema Society and Check4Cancer

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom




