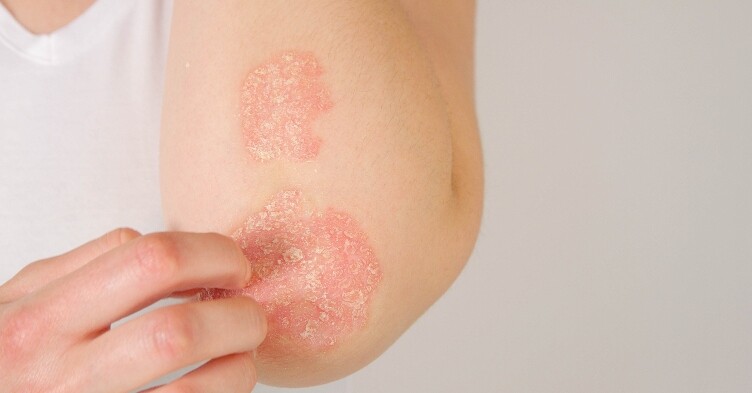
Blog: Topical corticosteroids – why the fear?

Topical corticosteroids (TCS) are the first choice for many inflammatory skin conditions such as eczema and for may patients and health care professionals (HCP) there is a fear and confusion about their use, side effects and long-term use. This is commonly known as ‘steroid phobia”.
The treatment has been around for many years, and the side effects often exaggerated; with concerns about skin thinning, general growth effects, alteration of skin pigment and increased hair growth. This means that patients and HCPs are often worried about using them when they are necessary and appropriate. It doesn’t help that there is often conflicting and confusing advice from different health professionals, pharmacists, friends, family members and the media.
Concerns about steroid strength are common and I often hear “I was told not to use too much as its really strong”. So do HCPs have an understanding of the strength (potency) of steroids applied the skin, how much to use, duration of use, type of product used and how to monitor their effect and side effects?
TCS are classified by potency: mild, moderate, potent or very potent and we should use these terms with our patients. If we don’t, patients often focus on the % of the TCS or name of products. The examples below show how the confusion can arise, with Hydrocortisone 1% Mild and Betnovate 0.1% Potent.
Potency examples
Related Article: Abdominal body fat is a higher risk for developing psoriasis
Mild – Hydrocortisone 1%
Moderately potent – Clobetasone butyrate 0.05% (Eumovate)
Potent – Betamethasone 0.1% (as valerate) (Betnovate)
– Hydrocortisone butyrate (Locoid)
Very potent – Clobetasol propionate 0.05% (Dermovate)
The potency of the preparation is the result of the formulation as well as the corticosteroid within it. This week whilst writing this blog I was contacted by a one of my families. I had prescribed a potent TCS ointment and the GP had issued a repeat of the TCS but as a cream rather than ointment. They were concerned that the cream was stronger again looking at % and this is a question I am commonly asked.
“Both are Cutivate (fluticasone propionate) but the one from the hospital is 0.005% w/w ointment whilst the one from the GP is 0.05% w/w cream.”
“By my calculations it appears that one is a lot stronger than the other. Can you clarify which is the correct strength please?”
Both are classified as potent but ointments penetrate the skin better than a cream hence why they are the same potency and the % varies. Also unless we specify an ointment, lotion or cream creams are issued by default. In addition to this we confuse our patients further with products prescribed / issued with a brand name or generically and expect them to tell us what products they are using. Asking patients to bring the products they are using with them is useful.
Related Article: CPD: Case by case – acute and emergency dermatology presentations
Other issues to consider when prescribing TCS include the duration of treatment, site of application, whether they are occluded (under plastic, dressings, bandages) and the words we use such as “use sparingly and thinly” which evoke anxiety. These issues will impact on the therapeutic effect and potential side effects. Inappropriate use will result in side effects and appropriate use will have a beneficial effect.
Monitoring quantities used and providing written advice; about the potency, formulation, site of application, duration and quantities are the fundamentals of TCS education. This should be supported with further information regarding the conditions to be treated, response to the treatment and any risks/ side effects or potential complication both from the products used on the skin or the skin condition itself.
Further Information
BAD (2016) Patient Support Groups:
http://www.bad.org.uk/for-the-public/patient-support-groups
BAD (2015) Topical Corticosteroids. http://www.bad.org.uk/shared/get file.ashx?id=183&itemtype=document
Related Article: Mythbuster: ‘This patient’s ulcer swab is positive so they need antibiotics’
Electronic Medicines Compendium (eMC): https://www.medicines.org.uk/emc/about-the-emc
NICE BNF Formulary (2014) Topical Corticosteroids: http://www.evidence.nhs.uk/formulary/bnf/current/13-skin/134-topical-corticosteroids
Patient (2014) Fingertip Units for Topical Steroids: http://patient.info/health/fingertip-units-for-topical-steroids

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom


Topical corticosteroids (TCS) are the first choice for many inflammatory skin conditions such as eczema and for may patients and health care professionals (HCP) there is a fear and confusion about their use, side effects and long-term use. This is commonly known as steroid phobia”.