Excessive scarring associated with range of conditions and ethnicity, study finds
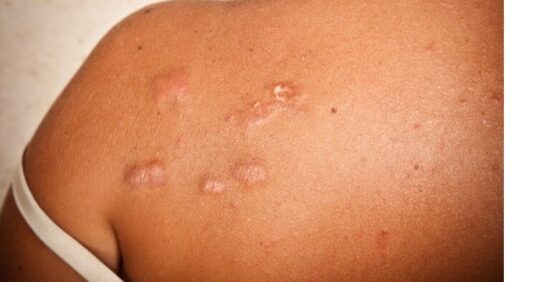
Excessive scarring, known as keloid and hypertrophic scars, is particularly associated with several co-morbidities, including atopic eczema, hypertension, musculoskeletal diseases and pain, a new study has found.
Researchers at King’s College London discovered the link in a recent analysis of UK Biobank data. They believe the association occurs because excessive scarring may share underlying predispositions with systemic diseases.
Related Article: Diagnosis Connect service will link people to advice from charities
The likelihood of developing these conditions was also found to be linked to a person’s ethnicity, with hypertension and fibroids more commonly seen in Black people with excessive scaring.
The findings were published in JAMA Dermatology.
Excessive scarring, known as keloid and hypertrophic scars, is a disfiguring chronic skin condition that is hard to treat and, according to the researchers, is relatively understudied. The scars are caused by excessive collagen production, are often painful and itchy, and can cause movement problems around joints. Keloid scars can continue to grow beyond the edge of the wound, whereas hypertrophic scars are contained at the site of the original wound.
Using medical records from the UK Biobank, the researchers investigated co-morbidities associated with keloid and hypertrophic scars. In a sample of 972 people who had excessive scarring and a control population of over 200 000, they found an association between scarring and atopic eczema and hypertension, which varied with ethnicity. Vitamin D deficiency was found to be associated with excessive scarring in Asian participants.
Related Article: CVD prevention must be national health priority, says report
In addition, previously unreported non-dermatological associations were found, including musculoskeletal disease and pain symptoms.
The researchers stated that the occurrence of multiple conditions hints at a common mechanism between excessive scarring and co-morbidities. With further research, visible skin scarring could help with early identification and even prevention of internal issues that are associated with the external condition, they suggested. The work also highlights ethnic variations in disease incidence.
Related Article: Postnatal contraception advice reduces the risk of back-to-back pregnancies
Dr Chuin Ying Ung, the lead author of the study, said: ‘Our study highlights the breadth of valuable information that can be gained from studying UK Biobank data. However, we also observed important gaps in current electronic health records, which, if addressed, would benefit wider research in dermatology and beyond.’

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom




