How to manage the inflammatory skin disease erythroderma
This article on how to manage erythroderma was first published by Nursing in Practice’s sister title Pulse as part of its non-Covid clinical crisis series.
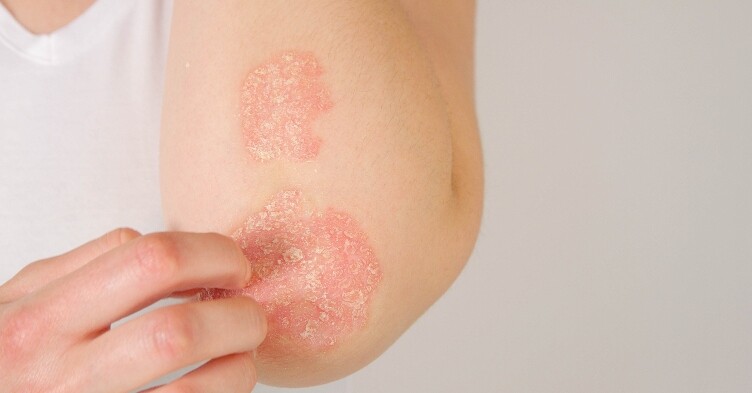
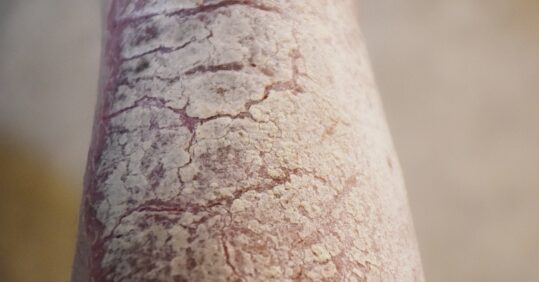
Erythroderma is generalised skin failure with widespread erythema over 90% of the body surface area where skin becomes red and can be intolerably itchy.
It usually develops quite rapidly but can come on gradually over several days or even weeks (especially with psoriasis). These patients can become ‘ill’ quickly, especially if they have co-morbidity. Ideally, GPs should always discuss the patient with a dermatologist on the phone or by email as the patient may need admission.
It is most often caused by:
• Eczema – especially atopic (more common in children and young adults)
• Psoriasis
Related Article: Call for regulatory guidelines as NHS adopts AI in dermatology care
• Drugs, most commonly sulphonamides, gold, carbamazepine, antimalarials and phenytoin. Typically comes on within first few weeks after introduction.
• Rarer skin conditions (eg, cutaneous T-cell lymphoma)
• Idiopathic (30% cases no cause found)
How to manage erythroderma
1. Review and consider stopping anything non-critical medicines. Start general vitamin supplements, especially vit B vitamins and folic acid, early as patients can rapidly become malnourished as ‘ill’ and likely to have increased need at time of reduced nourishment.
2. To prevent heat loss, maintain a warm and humid ambient room temperature at all times. May need to monitor for hypothermia. Ideally acquire a low reading thermometer and check at least daily
3. The skin barrier has failed, so water loss can be dramatic. Warm, wet towels (very regularly changed) may be needed. Encourage regular fluids and at least an additional 1-2 litres fluid a day. May need salty foods. Caution – This condition can cause high output heart failure with marked postural hypotension (warn patient and carers)
4. Check baseline bloods including FBC/CRP/U+E /LFT (with albumen) etc. Getting bloods done may be difficult at present, but electolytes, especially sodium and potassium, can become deranged if the patient is losing fluids from their skin.
5. Regularly smooth on an emollient of the patient’s choice possibly up to every couple of hours. The emollient be stroked gently down body and limbs and a 500g per week supply will be needed as a minimum. Good options include Hydromol ointment, Adex, and Emollin spray
Related Article: Abdominal body fat is a higher risk for developing psoriasis
6. Wash with a warm wet sponge using an emollient and no detergents
7. Encourage mobilisation to reduce the risk of DVT and bed sores. Provide sheepskin if possible
8. Watch for signs of skin infection, such as pain, serous ooze becoming crusty, and fever. Oral antibiotics may need to be prescribed early
9. If skin is oozing a lot, it can cause hypoalbuminaemia and a healthy, high protein diet should be encouraged
10. The itch can be intolerable and a mild or moderate potency topical steroid, such as clobetasone butyrate (eumovate) could help and should be applied once a day and half an hour away from applying any emollient. The patient may need 200g or more a week and lotions may be easier. Antihistamines, eg hydroxyzine, may also help with itc, but if not, then their only benefit is sedation.
11. Abrupt steroid withdrawal – oral or topical – can trigger an erythrodermic crisis in patients with previously stable psoriasis. This can even become generalised with painful sterile pustules just below the stratum corneum (so they rupture easily). Discuss with dermatologist
12. If the underlying condition is known, specific treatment for that would help, however:
Related Article: CPD: Case by case – acute and emergency dermatology presentations
• Avoid vitamin D analogues for erythrodermic psoriasis
• Avoid a topical immune-modulator in erythrodermic eczema
• Consider systemic treatments (e.g. oral steroids for eczema or methotrexate for psoriasis) but this should be discussed with a dermatologist as neither ideal during COVID-19 pandemic. If you can’t speak to a dermatologist, the dose would depend on the patient’s general condition and severity of erythroderma in order to manage it. But typically, 20-4-0mg/day for seven days, carefully monitored if possible (glucose / U+E) as well as the skin condition for response and tapered off as appropriate.

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom