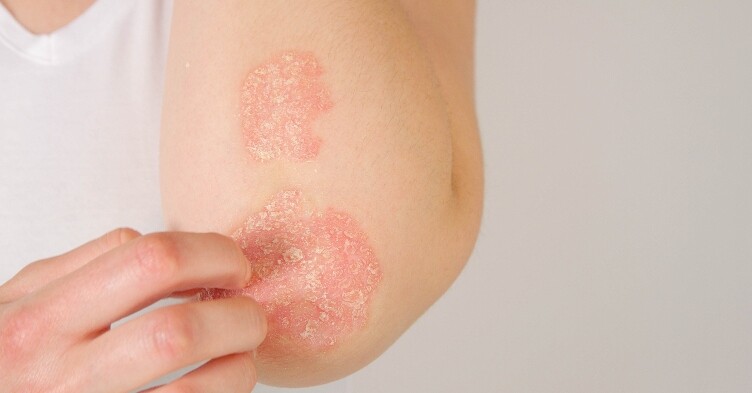
Infant atopic eczema – how health visitors can support parents and carers
Key learning points:
– Health visitors are key health professionals who can recognise symptoms of atopic eczema early
– First-line management is complete emollient therapy and topical steroids for
short-term flare
– Parent and carer support and practical information will help prevent severity and family distress
Atopic eczema is a very common skin condition that affects 20% of children in the UK and is increasing year on year.1 It generally presents in infancy, with 60% of all child sufferers developing it in the first six months of life1.
In the course of their daily work, health visitors frequently examine infants’ skin and will observe signs and symptoms that may indicate atopic eczema is developing. They have an essential role in providing advice, supporting parents and carers and helping them with individualised skin care.
The information in this article is presented as common questions from parents; the answers are professional evidence-based commentary.
What is atopic eczema?
Atopic eczema is a chronic condition with abnormal regulation of the immune system and primary functions of the epidermis (stratum corneum). Atopy is genetic and is responsible for eczema, asthma and rhinitis. Atopic eczema involves a complex interaction between the environment and genes, which leads to skin barrier dysfunction (due to the mutation in the skin matrix protein filaggrin, which is a key feature of atopic eczema) and local systemic immune dysregulation.2 Allergens and environmental allergies are also related to all atopic conditions, and an overactive immune response to environmental factors, contributing to eczema flares.2
Why does eczema develop before asthma?
The atopic march describes the development of atopic diseases, beginning with a family history and usually commencing in infancy or childhood with the development of atopic eczema and IgE-mediated food allergy; then in childhood asthma and rhinitis.3 Skin barrier dysfunction is the first step in the atopic march and inter relationships between atopic diseases can be explained by genetic risks, such as the mutation of filaggrin. The role of an atopic immunologically dysfunctional skin barrier is likely to be central to the evolution of allergic responses, including food allergy in atopic patients with relevant environmental exposure.3
Why is skin dry, red and itchy?
The abnormal epidermal function and changes in filaggrin alter protease and protease inhibitors, reducing the levels of natural moisturising factors (NMFs) by up to 80%, which causes dry skin due to the breakdown of the skin barrier.4 NMFs play an important role in regulating surface skin pH. A reduction in NMFs affects the acid mantle of the skin, which is enhanced by environmental triggers such as soaps and detergents.
In order to visualise skin barrier breakdown, imagine a brick wall with crumbly mortar and broken bricks, open to the elements and unable to remain waterproof.4
Atopic eczema is a complex disease with many immunological features. Flares may be caused by Langerhans cells, inflammatory dendritic epidermal cells and plasmacytoid dendritic cells, leading to interaction and release of inflammatory cells, T-cell priming, and cytokine and chemokines.
How do you know if an infant has atopic eczema?
Many infants will have transient skin conditions from birth, and atopic eczema can also develop in neonates. Generally, the first type of eczema to develop in infants is seborrhoeic dermatitis (cradle cap), which is self-limiting and resolves around six months. Atopic eczema usually develops on the face, where it can be severe, often wet and weepy (sometimes infected); and with generalised patches on the body. Often the nappy area is spared. In skin types IV and V, skin signs and symptoms can differ with follicular patterns and pigmentary changes, hypo and hyperpigmentation (erythema may not be visible), and, when the infant is over one year, reverse flexural pattern affecting extensor areas.5 Table 1 gives the current UK guidance criteria for diagnosis.
Related Article: Abdominal body fat is a higher risk for developing psoriasis
What is responsible for causing eczema or making it worse?
Parents and carers need to understand that atopic eczema is a multi-factorial condition. There is never one single cause; there are many actual, potential and individual trigger factors. Exposure to one or more environmental triggers will develop and exacerbate eczema in infants. This is why allergy testing in infants is not offered routinely, with the exception of IgE and RAST tests for suspected severe allergy, and the double-blinded placebo controlled food challenge (DBPCFC) which is commonly undertaken in children up to three years of age.6
Atopic eczema has many triggers, including:
– Soaps and detergents.
– Irritants (wool and synthetic clothing, perspiration, disinfectants, topical antimicrobials).
– Contact allergens (preservatives in topical medications, perfume-based products, metals and latex).
– Inhalant allergens (house dust mite, animal dander, cockroach, tree/grass pollens and mould).
– Environmental factors (hard water, cooking with gas).
– Family factors (genetics, teething, psychological factors and lack of sleep).
– Food.7
Is diet the cause?
Food allergies can be IgE mediated:
– Type 1, in which there is an immediate reaction
– Type 2, which occurs more than two hours after exposure and is mediated by cellular mechanisms without involvement of IgE.6
The cumulative incidence of IgE-mediated food allergy was 2.6% with 2.1% reacting to hen’s egg. For non-IgE-mediated food allergy the cumulative incidence was 2.4% (cow’s milk 1.7%), in all children and atopic eczema is a risk factor for developing food allergy.8 Sensitisation to food allergy occurs when there is exposure via a defective skin barrier, before immune tolerance has occurred after exposure through the gut. When a food allergy develops, this triggers an immune reaction on each exposure.
In general, food allergy presents at around three months old and below two years. The vast majority is limited to nine food groups: milk, egg, peanut, soya, wheat, tree nuts, sesame, shellfish and kiwi fruit.6
Diagnosing food allergy in children up to three years of age is based on clinical history and DBPCFC6 and infants with suspected food allergy should be referred to a paediatric dermatologist or allergist. Parents should not attempt their own exclusion diets as this may affect the infant’s growth and development.
Can eczema be prevented in infants?
Infants who are predisposed to atopic eczema, by inheritance of the atopic gene and genetic mutation of filaggrin, need appropriate skin care from birth, to try to reduce the likelihood of skin barrier breakdown and potentially the development of atopic eczema. The Barrier Enhancement for Eczema Prevention (BEEP) research study is looking at whether using skin barrier enhancement intervention (emollients for moisturising and soap substitutes for washing) can prevent eczema from developing.9 Recent evidence has shown breastfeeding is not linked to preventing eczema; and there is no evidence to support the health claim approved by the US Food and Drug Administration (FDA) that a partially hydrolysed formula could reduce the risk of eczema.10
How can eczema be treated?
The most important treatments are emollients as ongoing daily management and topical steroid for short-term treatment for flares.
Topical corticosteroids are effective in reducing inflammation and should be prescribed as first-line treatment for acute flares in infants. The National Institute for Health and Care Excellence (NICE)7 recommends the most effective preparation should be chosen for the area of the body and severity of eczema. Dilution should be avoided. Infants are generally treated with mild topical corticosteroids. Ointment preparations are used when skin is dry and creams are used when areas are wet and weepy. Moderate or potent topical steroid may be required for short-term treatment of more severe eczema, generally under the supervision of a dermatology specialist. NICE gives clear guidance for topical steroid treatment in children by using a stepped approach, which matches topical steroid potency to the age of the child, eczema severity and body site.7 Topical corticosteroids should be applied in therapeutic amounts for short bursts of treatment (up to one week and then reviewed). The ‘use sparingly’ direction usually leads to under-use and inadequate treatment. Parents and carers are frequently concerned about the potential side-effects of topical corticosteroids, which occur only if used incorrectly or excessively.11 The most common side-effects are localised to application sites; atrophy is a concern, as it may become permanent. The risk is also dependent on the potency of the topical corticosteroid, the degree of penetration (body site and occlusion), the extent of area treated and daily volume.12

Why are moisturisers (emollients) so important?
Emollients treat dry skin by providing a surface film of lipids, increasing water in the stratum corneum, which restores barrier function, and helps prevent the entry of environmental agents or triggers.13 Emollients soften the skin and reduce itch. Used regularly to maintain skin hydration, they can reduce the frequency of flares and be steroid sparing.13 Leave-on emollients may be lotions, creams, ointments or gels; they have either occlusive or additional humectant action. Emollients with occlusive effects trap water within the stratum corneum and reduce epidermal water loss. This effect may last for a few hours with emollient creams or longer with grease-based emollients.13 Humectant emollient creams contain NMFs and can produce similar rehydration as grease-based emollients with a higher degree of cosmetic acceptability.13
The emollient chosen for the infant should prevent dry skin and not cause irritation. Sometimes several products may need to be tried. Leave-on emollients should be applied regularly throughout the day, ideally at every nappy change and after bathing. They should be used liberally (infants require 250g/week), smoothed into skin in a downwards stroking motion and not rubbed in.
Related Article: CPD: Case by case – acute and emergency dermatology presentations
How often should infants with eczema be bathed?
Bathing is soothing for many patients but should always be with emollients and not soaps or foaming washes. Daily baths are recommended for infants with atopic eczema, as documented in a forthcoming study.
Very dry skin requires hydration with daily baths followed by moisturiser, a gentle pat-dry, then the immediate application of a moisturiser to seal. This process is known as ‘soak and smear’.14 Leave-on emollients can be used for washing (as soap substitutes) and applied after washing. An emollient is able to provide skin cleansing and is helpful in reducing Staphylococcus aureus. Dispersing bath oils are an option for complete emollient therapy but do not maintain skin hydration, so emollients need to be applied immediately after bathing, to maintain hydrating effect.
What if the eczema does not get better with treatment?
Infants whose eczema flare does not resolve with topical treatments recommended by NICE7 should be referred to a dermatology specialist. If allergy is strongly suspected they should be referred to an allergist or joint dermatology and allergy service.
Atopic eczema is frequently infected with s.aureus, as the skin of people with eczema has larger colonies of the bacteria. Antiseptic emollients (bath oils, washes and ‘leave-on’ emollients) are a helpful adjunct for decreasing bacterial load. In cases of recurrent infected eczema, once-twice weekly use is advised to help reduce S. aureus on skin7. NICE recommends that children with S. aureus-infected eczema should be treated with a one-to-two-week course of systemic antibiotics. Localised areas of bacterial infection can be treated with topical antibiotics or antibiotics combined with topical steroids for a maximum of 14 days.7 Bacterial resistance is an ongoing issue. NICE advises health professionals to be aware of this and to follow local guidelines for advice on patterns of bacterial resistance to antimicrobials (including antibiotic stewardship).7
Is there a patient support group?
The National Eczema Society (NES) is a UK charity providing support and information for people with eczema, parents and carers of children with eczema and healthcare professionals. Parents and carers can contact the NES on the helpline (phone call or email) to talk to someone or ask questions; and the NES provides booklets and leaflets to help them understand more about coping with and managing their child’s eczema. The NES also has a dedicated area on its website for healthcare professionals to download information and news on training days around the UK. The website is eczema.org and the helpline is 0800 089 1122 (08.00-20.00 Monday-Friday) or email [email protected]
Conclusion
Emerging research is focusing on eczema prevention, so early recognition and treatment in infancy is essential. Health visitors are well placed to take on and expand this role.
References
1. Irvine AD, McLean WH, Leung DY. Filaggrin mutations associated with skin and allergic diseases. New England Journal of Medicine 2011;365(14):1315-27.
2. Schofield J, Grindlay D, Williams H. Skin Conditions in the UK: a Health Care Needs Assessment. Centre of Evidence-Based Dermatology, University of Nottingham 2009;6:85-88.
3. Shaker M. New insights into the allergic march. Current Opinions in Paediatrics 2014:26(4):516-520.
4. Cork MJ, Robinson DA, Vasilopoulos Y. Epidermal barrier dysfunction in atopic dermatitis. Journal of Investigative Dermatology 2009;129:1892-1908.
5. Kelly AP, Taylor SC. Atopic eczema and other eczema’s.In Dermatology for Skin of Colour 2009;27:163-167.
6. Beattie PE. Adverse food reactions in patients with atopic eczema. Dermatological Nursing 2015;14(2):10-14.
7. NICE. Atopic eczema in children. nice.org.uk/CG57 (accessed 5 July 2016).
Related Article: Mythbuster: ‘This patient’s ulcer swab is positive so they need antibiotics’
8. Grimshaw KE, Byant T,Oliver EM. Incidence and risk for food hypersensitivity in UK infants: results form a birth cohort study. Clinical Allergy 2016;26(1). DOI: 10.1186/s13601-016-0089-8.
9. Simpson EL, Hanifin JM, Thomas KS. Barrier enhancement f the skin barrier from birth offers effective atopic dermatitis prevention. Journal of Allergy and Clinical Immunology 2014;134(4):818-23.
10. Boyle RJ, Lerodiakonou D, Khan T. Hydrolysed formula and risk of allergic or autoimmune disease: a systematic review. British Medical Journal 2016;8(352). DOI: 10.1136/bmj.i974.
11. Arden-Jones MR, Flohr C, Reynolds NJ, Holden CA. Atopic Eczema.In Rook’s Textbook of Dermatology 2016;41:27.
12. Long CC, Finlay AY. The fingertip unit: a new practical measure. Clinical Experimental Dermatology 1991;16:444-7.
13. Cork MJ, Danby S. Skin barrier breakdown: a renaissance in emollient therapy. British Journal of Nursing 2009;18(14):872-7.
14. EureckAlert. Daily soak and smear, 2016. eurekalert.org/pub_releases/2016-06/acoa-da062316.php (accessed 6 July 2016).

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom


Atopic eczema is a very common skin condition that affects 20% of children in the UK and is increasing year on year