NICE planning expansion of diabetes continuous blood glucose monitoring devices
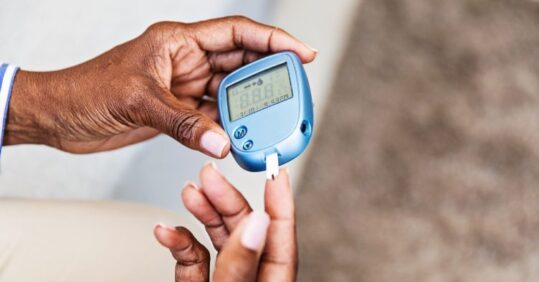
NICE has consulted on recommendations to dramatically expand access to continuous blood glucose monitoring devices to all adults with type 1 diabetes and some with type 2 disease.
Under the proposals patients with type 1 diabetes would have a choice of a real-time continuous glucose monitor (CGM) device or flash monitor ‘based on their needs and preferences’.
Flash monitors that offer intermittent CGM should also be offered in adults with type 2 diabetes on multiple daily insulin injections if they have recurrent or severe hypoglycaemia, impaired hypoglycaemia awareness or have a condition or disability that means they cannot self monitor their blood glucose.
These patients could also be offered real-time CGM devices if available for same or lower cost, the update to NICE type 2 diabetes management guidelines says.
Related Article: Research insights: the latest updates from clinical papers
All patients using flash or real-time monitoring devices should be managed by ‘a team with expertise in its use’, NICE said. The consultation is open until 22 December and final guidance on both is expected next year.
The draft update also warns clinicians not to use age or body mass index alone to exclude or diagnose type 1 diabetes and to keep in mind the possibility of other diagnoses.
In adults with an initial diagnosis of type 1 diabetes, diabetes-specific autoantibody test should be done and serum C-peptide should not be routinely used to confirm a type 1 diagnosis, NICE said.
Technology guidance from NICE on use of integrated pump systems in managing diabetes is also in the process of being updated and will include assessment of hybrid closed loop systems.
Figures from NHS England show that half of type 1 diabetes patients – around 125,000 with the condition – are now using flash monitors to check their blood glucose levels.
The original target in the NHS Long Term Plan was for 20% of people with type 1 diabetes to have flash monitors by March this year.
Dr Partha Kar, NHS England’s national specialty advisor for diabetes, said: ‘The high uptake in people with Type 1 diabetes is a clear example of the NHS’ commitment to improving care for people living with this condition and it’s down to the hard work of NHS staff that we’ve managed to roll these out at such a pace, smashing our target of offering to 20% of those eligible by March.
Related Article: Half of women with gestational diabetes report facing stigma
‘I am delighted that NICE has started consulting on wider use of the technology and we thank them for working with us on this. We look forward to implementing the final recommendations from NICE, following the consultation period.’
Dr Becky Haines, a GP and clinical lead for diabetes at NHS Newcastle Gateshead CCG, told Pulse: ‘It is amazing news for people with diabetes who can benefit from these life-changing technologies but it’s going to need extra resources in either secondary or primary care, or more likely a mixture of both.’
She noted that current initiation of CGM and flash devices was mainly done in secondary care who have expertise and access to the software for monitoring them once people are using them.
‘So, either we will need to refer more people into diabetes services or practices will need to upskill and be funded to do this work,’ she said
She added: ‘Many practices will be caring for people with type 2 diabetes on insulin, currently with no secondary care input. They will either need to be referred into local diabetes services, or initiation of flash will need to be transferred to primary care with appropriate funding and training.’
Related Article: Type 2 diabetes treatment updates: putting NICE into practice
To complete relevant diabetes modules on Nursing in Practice Learning, click here.
A version of this story was originally published on Nursing in Practice sister publication Pulse.

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom




