Patterns and trends in eczema management in primary care
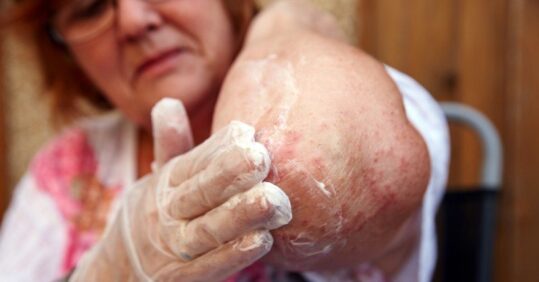
Eczema is the most common inflammatory skin condition in children worldwide, and one that often continues into adulthood. The condition can be incapacitating and patients of all ages can experience a psychological impact. Management is led by primary care, and attendance rates are high: 96% of children with eczema have had a primary care attendance in the preceding year.
In their study1, de Lusignan and colleagues (2021) used a large primary care research database to assess healthcare use and treatment patterns among people in England with new onset of active eczema (n = 411,931) between 2009 and 2018.
Related Article: ‘Patients not prisoners’: Palliative care nursing behind bars
Primary care consultation rates increased from 87.8 per 100 person-years to 112.0 per 100 person-years over that period, while specialist referral rates rose from 3.8 to 5.0 per 100 person-years. Primary care consultations were highest in children under two years of age, but referral rates were highest in over-50s. Socioeconomic discrepancies were observed: specialist referral rates were lowest in people of lower socioeconomic status despite their higher rate of primary care consultations.
The study period saw slight alterations in prescribing practice. Prescription of emollients increased for those with active eczema from 48.5% to 51.4%, while there was a decrease in prescribing of topical corticosteroids from 57.3% to 52%. People of non-white ethnicities and lower socioeconomic status were less likely to be prescribed potent topical corticosteroids.
Related Article: NHSE confirms dates and eligibility for autumn Covid and flu jabs
The authors said the disparities in eczema management warrant further study, in particular the lower rates of referral in those from more deprived backgrounds and the greater risk of progression to moderate and severe eczema in children of non-white ethnicity. The study’s main limitation was that inaccuracies in recording diagnosis dates mean onset for some patients may have occurred before the study period.
Lucille Kelsall-Knight is a lecturer in children’s nursing at University of Birmingham School of Nursing
Reference
Related Article: ‘Concerning acceleration’ in drug-resistant gonorrhoea ahead of vaccine programme
1 de Lusignan S et al. Patterns and trends in eczema management in UK primary care (2009–2018). Clin Exp Allergy 202;51:483–494. doi.org/10.1111/cea.13783

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom




