‘I have a sore throat – I need antibiotics’

Debunking common patient myths and misconceptions
The myth
Related Article: ‘Patients not prisoners’: Palliative care nursing behind bars
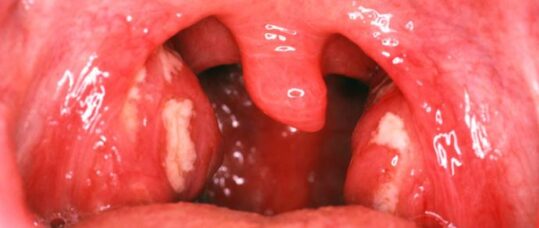
A painful sore throat means I have tonsillitis – particularly if there are white spots on my tonsils – and I need antibiotics.
The reality
Most sore throats are caused by a viral infection and don’t require antibiotics.
A sore throat is a common condition, with a third of adults reporting a sore throat and a third of those visiting the doctor each year.1 You should explain to patients that a sore throat is usually a self-limiting condition, with a 40% chance of recovery within three days and 85% chance within a week. Antibiotics will generally reduce the duration of symptoms by one day – but at the risk of side effects such as diarrhoea and thrush, as well as the risk of building up a resistance to the drug.
The NICE guidance says that ‘most people get better without antibiotics’ and ‘withholding antibiotics rarely leads to complications’,2 but it is still common for people to believe that a severe sore throat or flecks of white pus on the tonsils means that antibiotics are needed.
The severity of a sore throat can be assessed using either the Centor score or FeverPAIN (see box, right). NICE recommends using one or the other; in practice, they are essentially the same.
Even if a patient has a maximum score that doesn’t necessarily mean they require antibiotics. A maximum FeverPAIN score of 5 gives no more than a two-thirds chance that the streptococcus bacteria will be isolated from the throat. The Centor top score is even less, with 4 giving a 50-60% chance of a bacterial infection.
Most of the features of these score systems can be accessed without seeing the patient, which is useful for services that use phone triage. Over the phone, if a patient has no temperature or painful lumps in their neck and has a cough, they will not need antibiotics, even if they have white spots in their throat. Instead, they can be signposted to their local pharmacy, where they can combine over-the-counter analgesia, such as paracetamol or ibuprofen, with throat lozenges and analgesic throat sprays. There is little evidence for the use of these treatments but anecdotally they are useful.
Related Article: NHSE confirms dates and eligibility for autumn Covid and flu jabs
However, there are cases when a sore throat can be more serious and does require antibiotics if indicated by the FeverPAIN/Centor scores. For example, patients taking drugs that suppress the immune system, such as methotrexate, ciclosporin, mycophenolate (usually given orally), and injectable biologic drugs that often end in ‘mab’, such as infliximab and adalimumab. These patients hopefully should be aware that they are immunocompromised and should tell you this information.
The same may apply to patients who are on chemotherapy or have HIV, which isn’t well-controlled with antiretroviral drugs. Any patients taking carbimazole for hyperthyroidism, which can sometimes suppress the bone marrow so that there aren’t enough white blood cells to fight infection, and presents with a sore throat should have a full blood count taken.3
Complications from a sore throat are rare and the SIGN guidance states that antibiotics should not be given to prevent complications, specifically because there is no evidence that they prevent rheumatic fever, glomerulonephritis, quinsy, or infection spreading in the community.4
We have a responsibility to manage antibiotics wisely, or they may not be available for future generations.5 It is rare that a sore throat needs antibiotics and we should take an evidence-based approach to only prescribe if absolutely necessary.
| Methods to assess the severity of a sore throat |
|---|
|
FeverPAIN score – one point for each, maximum 5 Related Article: ‘Concerning acceleration’ in drug-resistant gonorrhoea ahead of vaccine programme
|
|
Centor score – one point for each, maximum 4
|
References
- NICE CKS: Sore throat – acute. London;NICE:2018
- NICE. NG84: Sore throat (acute): antimicrobial prescribing. London;NICE:2018
- BNF. Carbimazole. London;NICE:2018
- SIGN 117. Management of sore throat and indications for tonsillectomy. Edinburgh;SIGN:2010
- Davies S, Sugden R. What if antibiotics were to stop working? London:The King’s Fund

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom


Debunking common patient myths and misconceptions



