CPD: Reviewing patients with rheumatoid arthritis
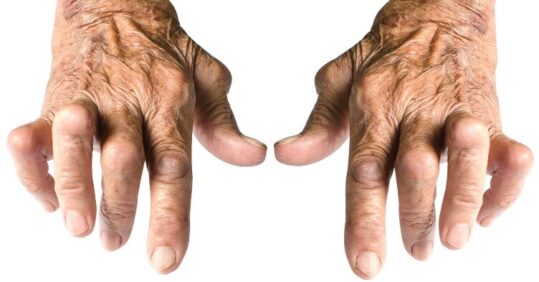
GP Dr Roger Henderson advises on what nurses in general practice need to be aware of when reviewing patients with rheumatoid arthritis
Module summary
Rheumatoid arthritis (RA) is a chronic autoimmune disorder that primarily affects the joints, although other organs may be affected. In autoimmune diseases like RA, the immune system mistakenly attacks the body’s own tissues, leading to inflammation in the affected areas. It is important in primary care for practice nurses to recognise potential signs and symptoms of RA, and understand the principles of managing RA when consulting patients diagnosed with the condition.
Related Article: Genetic link discovered between endometriosis and immune conditions
Learning objectives
By the end of this module, you will have a greater understanding of:
- The causes of rheumatoid arthritis.
- How it may present in patients.
- How rheumatoid arthritis is treated.
- The importance of regular monitoring and review.
- The prognosis for patients with rheumatoid arthritis.
What is rheumatoid arthritis?
Rheumatoid arthritis (RA) is a common chronic inflammatory autoimmune disease. It is characterised by joint inflammation and destruction, and is the most common form of inflammatory arthritis.1 Affecting around 1% of the UK population it is more common in women than men,2 and requires early and intensive treatment, to reduce the risk of significant morbidity arising from it, including joint damage but also problems affecting the lungs, heart, eyes and vasculature. People of any age may develop it but the peak age of onset in the UK is between 30 and 50 years old. If left untreated (or sub-optimally treated) it can significantly decrease quality of life, have an impact on employment, increase the likelihood of joint replacement surgery and increase overall mortality risk.3 The diagnosis is typically a clinical one, with further investigations such as imaging and blood tests providing prognostic rather than diagnostic information.
Related Article: How effective are non-surgical and non-invasive treatments for lower back pain?
What causes RA?
This remains unclear but it is thought there is a strong link to genetic susceptibility and environmental factors. The human leukocyte antigens HLA DR4 and DR1 are more common in patients with RA, especially in severe disease.4 Smoking appears to be an important risk factor5 with other possible environmental triggers being obesity, diabetes, and the presence of rheumatoid factor or anti-citrullinated protein antibodies in the blood.6 A possible link to infection has been suggested, although no particular organism has yet been identified. The onset of RA is also more common in the winter months, the reason for which is currently unknown.
To complete the full module visit the Nursing in Practice 365 website.
Related Article: Boost your CPD with the redesigned Nursing in Practice 365 platform
Dr Roger Henderson is a senior GP based in Scotland

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom




