Mythbuster: ‘I need to let the air get to this wound’
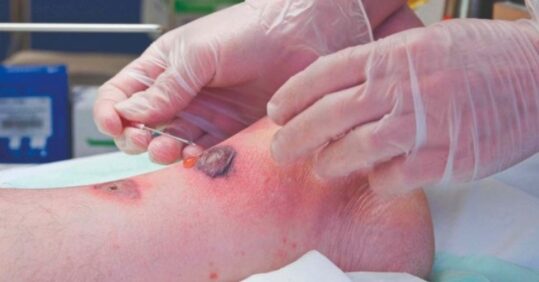
It is common for patients to suggest that their wound needs to ‘breathe’ and get air in order to heal. These thoughts often come from older family members citing that, for example, a child’s scabbed knee healed up without concern. But it is essential for the treating clinician to explain the importance of creating the right environment for wound healing for acute and chronic wounds based on the concept of moist wound healing established more than 50 years ago.1
Wound care in the UK carries a significant cost pressure for the NHS. The prevalence of wounds, inconsistencies in assessment of the wounds and the number of wounds contribute significantly to the burden on already overstretched health services.2
In 1962,1 Winter demonstrated that superficial acute skin wounds in pigs healed more quickly when covered with a film to create a moist environment, compared with wounds left exposed to air. This study evidenced that a moist environment encourages faster replication of epithelial cells and therefore faster wound healing. These epithelial cells migrate across a moist wound surface with ease, but a dry scab acts as a barrier to new cells trying to travel across the wound bed. This work has been widely cited in academic literature since it was first published. It is considered by wound care clinicians to be a seminal publication and will no doubt continue to be referenced.
There are of course some caveats for clinicians and moist wound healing may not always be the most appropriate plan of care for a patient. Clinicians should complete a holistic patient and wound assessment and then deliver the most appropriate option.
Related Article: Diagnosis Connect service will link people to advice from charities
The concept and delivery of moist wound healing may not be appropriate in the following instances.3 This is not an exhaustive list but provides examples to consider and explore further:
- Patients with a palliative diagnosis or those on a care-ofthe-dying pathway.
- Those with significant inoperable peripheral vascular disease with dry necrotic wounds.
- Diabetes patients with a dry necrotic toe that is being left to auto-amputate.
- Fungating wounds
- Wounds due to calciphylaxis
- Wounds due to meningococcal sepsis
- Necrotising fasciitis being managed palliatively and not with immediate surgery to save life or limb.
Since Winter’s original work was published,1 there has been a significant number of experimental and clinical studies providing further evidence that this method provides advantages for the patient. These studies were compiled into a table and published by Rippon, Ousey, Rogers and Atkin in 20164– you can view the full table and the breakdown of the evidence here. Some of the benefits of moist wound treatment listed include:
- Up to 50% faster wound healing
- Faster wound contraction
- Enhanced and faster reepithelialisation
- Generally increase cellular proliferation
- Prolonged presence of growth factors and cytokines
- Keratinocyte proliferation, fibroblast growth
- Promotes angiogenesis/ revascularisation
- Greater quantity and quality of ECM
- Collagen synthesis
- Lower rate of infection
- Cleansing/irrigation
- Painless removal of the dressing without destroying newly formed tissue
- Less scarring and better cosmetic results
- Enhanced autolytic debridement
- Decrease in initial donor site pain and improved donor site healing
Day-to-day practice
A small scab may initially develop at the site of a wounded area of skin as a natural result of the haemostasis phase of the healing process. Initially this may be of benefit to stem blood flow, but if left, this scab can become detrimental to wound healing, as discussed. Similarly, a focus on ensuring moisture is present at the wound bed can lead clinicians to make a wound too wet. This can also have a detrimental effect on the healing process, causing maceration on the wound edges and damaging the surrounding healthy tissue.4
A full patient and wound assessment allows for a plan of care based on the evidence and helps to prevent complications.
There is a wealth of products available in the UK via FP10 prescription and supply chain routes that support the concept of moist wound healing and allow a wound to be maintained in optimum conditions.
Final word
Related Article: CVD prevention must be national health priority, says report
As a tissue viability nurse specialist, I teach clinicians that if a wound is wet, they should dry it up. If it is dry, they should add some moisture. Tissue viability nurse specialists across the UK have developed formularies in clinical areas to assist clinicians in making an informed decision on wound care products that support the right healing environment, as well as adjunct therapies such as compression hosiery and bandaging, emollients, skin barrier film and cream protectors, debridement products. I encourage clinicians to familiarise themselves with the local formulary, so they are fully informed of the availability and use of all products. These products have been developed to facilitate faster wound healing, reduce pain, improve scar formation and improve quality of life for patients. It is important to choose them carefully and use them correctly.
If a wound is not infected, leaving a dressing in place is better than changing it frequently. Minimise dressing changes by assessing the wound carefully and choosing a wound care product that can effectively manage the exudate.
Clinicians should also familiarise themselves with the products that are not recommended for wound care as they will not facilitate a moist environment and support wound healing – products such as tulle dressings, gauze and cotton wool.
Build your knowledge so you can share the wealth of evidence when you need to discuss wound management with patients – and also if you need to challenge outdated practices if they are suggested by other clinicians.
Amy Verdon is a clinical nurse specialist in tissue viability at University Hospitals Coventry and Warwickshire NHS Trust
Related Article: Postnatal contraception advice reduces the risk of back-to-back pregnancies
References
- Winter, GD. (1962) Formation of the scab and the rate of epithelialisation of superficial wounds in the skin of the young domestic pig. Nature. 193: 293-4
- Guest, J, Ayoub, N. McIlwraith, T. et al (2015) Health economic burden that wounds impose on the National Health Service in the UK. BMJ open 5 (12): e009283
- Gray , D. Acton, C. Chadwick, P. Fumarola, S. Leaper, D. Morris, C. Stang, D. Vowden, K. Vowden, P. Young, T. (2010) Consensus guidance for the use of debridement techniques in the UK. Wounds UK. 6 (4)
- Rippon, M. Ousey, K. Rogers, A. Atkin, L. (2016) Wound Hydration versus maceration: understanding the differences. Wounds UK. 12 (3) 62-68

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom


Tissue viability nurse specialist Amy Verdon on the importance of creating the right environment for wound healing, dispelling the myth that wounds need to ‘breathe’ in order to heal



