Mythbuster: patients with lymphoedema must be managed by a specialist service
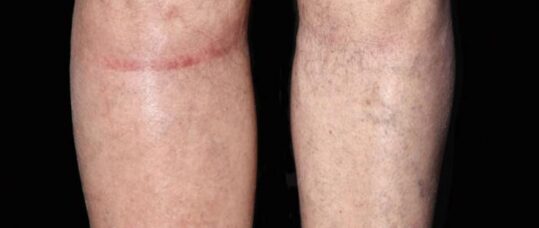
Nurse and lymphoedema lead Caitriona O’Neill on why managing lymphoedema is in the remit of the practice nurse
The myth
Lymphoedema can only be managed by a specialist service, as primary care nurses don’t have access to the right resources.
The reality
Practice nurses are essential in supporting long-term management of lymphoedema.
Lymphoedema sits under the umbrella term of chronic oedema, which is long-term oedema of the lower limb.1 The prevalence of chronic oedema is estimated to be four people in every 1,000, increasing to 29 people in every 1,000 over the age of 85.2
The long-term management can place a burden on health services, which has been well documented over recent years.3 The earlier that chronic oedema is identified, and appropriate management begins, the better the long-term outcome will be for the individual.
Once swelling has been present for some time, skin changes can occur and limb size increases, which can result in limb distortion, necessitating specialist management.
Related Article: ‘Patients not prisoners’: Palliative care nursing behind bars
Within primary care, the pathway for managing this group largely sits within community nursing or specialist lymphoedema services. Practice nurses are in a prime position to meet the provision for early intervention in the mobile groups; this is an area that is not routinely commissioned within community services, resulting in an unmet need.
There are three key areas to explore within the practice nurse setting:
- Early detection and management.
- Long-term maintenance.
- Health and wellbeing review.
Early detection and management
Early detection of chronic swelling prevents further complications; once management starts, there is an immediate reduction in complexities such as repeated cellulitis and skin changes in the lower limb.
Within general health reviews, lower limb swelling should be an essential component of the assessment. Once identified, consideration for the aetiology is required, and exclusion of any critical systemic concerns addressed and medically managed if appropriate.
Actively supporting management with simple non-complex swelling is advised. A key concern for practice nurses is the lack of ability to complete a full Doppler assessment as part of a vascular assessment, but there are several documents that can support a clinical vascular assessment in the absence of a Doppler completed in a systematic approach.
The suggested focus should be individuals that fall into the following groups:4
- Minor lower limb swelling.
- Early stage venous disease.
- Acute lower limb wound (pre-tibial laceration).
- Pregnancy – this should only be mild swelling (not moderate or severe).
Ensure patient meets all below criteria:
- Intact sensation.
- Good peripheral perfusion (no signs of limb ischaemia).
- No deep pitting or skin folds.
- Appropriate shape and size of limb (below knee measurement should not be significantly wider than the calf).
The British Lymphology Society5 supports this pragmatic approach in the absence of an ankle brachial pressure index (ABPI) measurement for patients who present with chronic oedema in the absence of significant cardiovascular risk factors and clinical signs or symptoms of peripheral arterial disease (PAD), provided the vascular status has been thoroughly assessed (see the table below). You can complete a checklist to identify any key risk factors (Vascular Assessment Holistic Tool).5 Clear documentation and communication of the rationale is essential.
Carrying out a full vascular assessment5
History and symptoms
- Recent and past medical history (diabetes, cardiac status, AF, previous cancer, DVT, stroke, hypertension, hyperlipidaemia).
- Surgical history (interventions on the arteries or veins).
- Cardiovascular risk factors (including smoking status).
- Medications.
- Symptoms – time of onset and clinical progression (improvement or deterioration) should be recorded:
- Intermittent claudication (often described as muscle pain on mild exertion, ache, foot or great toe pain, numbness or sense of fatigue, classically in the calf muscle, which occurs during exercise such as walking and is relieved by a short period of rest).
- Chronic ischaemic rest pain (usually described as night cramps, with an inability to lie in bed and a need to hang leg out or sleep in a chair).
- Acute ischaemic pain.
- Neuropathic or musculoskeletal pain.
Clinical examination
- Peripheral neurological status (motor or sensory deficit).
- Oedema (lipoedema, lymphoedema, pitting oedema).
- Peripheral pulse palpation (pulselessness).
- Skin colour (pallor or mottling in acute ischaemia, rubor or duskiness in chronic ischaemia).
- Nails (atrophic nail changes).
- Temperature (cooler at the extremities).
- Trophic skin changes (ulceration, pre-ulcerative lesions).
- Venous hypertension (varicosities, telangiectasias, eczema).
- Capillary refill (the time taken for colour to return to an external capillary bed after pressure is applied to cause blanching).
- Buerger’s test (elevating both legs 30-45 degrees for two to three minutes: in the case of ischaemia, pallor and delayed venous refilling can be observed).
If the criteria for early intervention are not met, or concern arises from clinical presentation or during holistic history-taking regarding arterial insufficiency, then onward referral can be sought to enable a full vascular assessment. If a lower limb wound is present, this should also trigger onward referral if it’s not healing after two weeks. To prevent delay in management, prescribe class 1 British standard hosiery (max 17mmHg compression) in the absence of ABPI.
Related Article: NHSE confirms dates and eligibility for autumn Covid and flu jabs
Long-term maintenance
Exit pathways are essential for specialist services to be sustainable and effective. It is a long-term condition that requires lifelong management, and specialist services have an interdependency on other providers in community nursing (housebound patients) and primary care (mobile patients). The key components of long-term management require intermittent review of progress to ensure that any hosiery garments provided on repeat continue to be suitable, and that the management plan outlined has been followed.
Key medical concerns should be identified as the treatment plan may need review. In some cases, this may require a re-referral to the specialist services if complexities are identified.
Health and wellbeing review
The key components to lymphoedema/chronic oedema management are:
- Skin care.
- Compression.
- Exercise.
These core components should be reviewed alongside general health and wellbeing, with a focus on embedding an understanding of the condition while promoting selfmanagement. Obesity and dependency (oedema occuring in the lower half of the body) are two critical issues that will limit management. It is essential for a weight-management plan to be followed to reduce the burden on the lymphatic system. When we generally speak about dependency in a community setting, this relates often to the issue of not sleeping in bed. In mobile patients, dependency can be affected by ill-fitting, unsecure footwear, resulting in poor gait and reduction in the calf muscle pump efficiency.6 Routine health reviews should highlight these concerns, which can be addressed with weight management and optimum exercise being supported and promoted.
Summary
Management of long-term conditions is in the remit of the practice nurse and chronic oedema is one of these conditions. Integration of pathways for this complex group is essential, from early intervention to long-term management.
Related Article: ‘Concerning acceleration’ in drug-resistant gonorrhoea ahead of vaccine programme
Practice nurses have the opportunity to support transformation within primary care for early recognition of lower limb oedema and be proactive in management and enabling self-care. The barriers to prescribing compression hosiery without an ABPI can be overcome with clinical assessment using the vascular assessment tool, or by ensuring there is a diagnosis and that essential criteria have been met to support decision-making in hosiery application. Much can be achieved with a simple holistic assessment and embedding of lower limb review within primary care.
Caitriona O’Neill is a nurse and the director of community services and lymphoedema lead at Accelerate CIC, a social enterprise that works in the NHS to deliver specialist care to patients with chronic wounds and lymphoedema
References
- Watts T. Four Cornerstones of Lymphoedema Care. Nursing and Residential Care 2018;20:310-18
- Moffatt C, Keeley V, Franks P et al. Chronic oedema: a prevalent problem for UK health services. Int J Wounds 2017;14: 772–81
- Moffatt C, Gaskin R, Sykorova M et al. Prevalence and risk factors for chronic oedema in UK community nursing services. Lymphatic Research and Biology 2019;17:147-54
- Wounds UK. Best Practice Statement: Holistic Management of Venous Leg Ulceration. 2016
- British Lymphology Society. Position paper for ankle brachial pressure index 2018 thebls.com/public/uploads/ documents/document- 20621539855354.pdf
- Farrelly I. Ten top tips: improving mobility in people with wounds. Wounds International 2017;8:14-18

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom


Nurse and lymphoedema lead Caitriona O’Neill on why managing lymphoedema is in the remit of the practice nurse



