Treatments for patients with acne
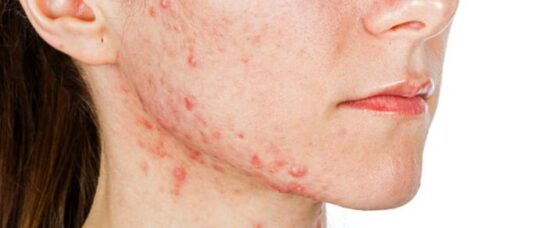
Effective management of acne requires support and should include practical realistic advice about caring for the skin.
It must address individual concerns and expectations about the treatment options, which will impact on treatment adherence.
The focus should be to treat without delay, to reduce or clear skin lesions with minimal side effects, to prevent physical and emotional scarring, and reduce antibiotic resistance.1
The Primary Care Dermatology Society’s 2018 guideline provides a comprehensive overview of the aetiology, clinical findings and images, investigations, and management of acne (see resources).
Related Article: Diagnosis Connect service will link people to advice from charities
Topical therapies should be the first option for treating acne. It is essential that topical therapies are applied correctly and regularly. Initial application may cause irritation and dryness, therefore short contact (eg 30 minutes followed by washing off), and gradually increasing the frequency and duration will help to aid tolerability. Products must be applied to all acne-prone areas rather than just specific lesions to prevent follicle development.2
Mild to moderate acne should be treated topically with preparations containing benzoyl peroxide or topical retinoids, such as:
- Adapalene (Differin).
- Adapalene combined with benzoyl peroxide 2.5% (Epiduo).
- Isotretinoin (Isotrex).
Mild to moderate papular or pustular acne should be treated with a combination treatment, ideally containing benzoyl peroxide, which reduces bacterial resistance, with either a topical retinoid or topical antibiotic:
- First line: Epiduo gel (adapalene with benzoyl peroxide).
- Second line: Duac gel (clindamycin with benzoyl peroxide).
- Other options: Treclin gel (clindamycin and tretinoin) and Erythromycin combinations – Aknemycin Plus solution or Isotrexin gel.
If patients are not responding to the above or the acne is more widely distributed, the combination of a systemic antibiotic and an appropriate topical agent, preferably benzoyl peroxide (or a topical retinoid if benzoyl peroxide is not tolerated) to reduce bacterial resistance may be required.
There are, however, increasing levels of Propionibacterium acnes resistant to antibiotics, especially erythromycin, the use of which should be restricted.
Generally, Lymecycline 408mg OD (Tetralysal) daily for three months is the antibiotic of choice as compliance is good (it can be taken with food) and bacterial resistance is less than with first generation tetracycline’s.
Related Article: CVD prevention must be national health priority, says report
Other options may include doxycycline and rarely minocycline.
Macrolides should generally be avoided in adults due to high levels of P.acnes resistance but may be used as first line in pregnancy and children under the age of 12 as tetracycline’s are contraindicated.
Trimethoprim may be used for young children who do not tolerate macrolides but again there are concerns with bacterial resistance. In women with moderate to severe acne, adding in Dianette to the topical or systemic treatments may be considered.3 Patients with severe disease and poor prognostic risk factors should be referred for consideration of isotretinoin. Isotretinoin is licensed as a second-line therapy for acne that has not responded to combination regimens including antimicrobials and topical retinoids.4
Other treatments include over-the-counter products (see Table 1) and procedures such as laser therapies, chemical peels, and steroid injections, which should only be undertaken by a trained professional.5
| Table 1: Over-the-counter treatments5 | |||
|---|---|---|---|
| Product | What is it? | How does it work? | What are the side effects |
| Tea tree oil | Tea tree oil is an essential oil. A product that is designed to be applied to the skin and not raw tea tree oil should be used as can be a skin irritant. | Tea tree oil acts as an anti-inflammatory and is less irritant to the skin than benzoyl peroxide. Tea tree oil is also anti-bacterial. | Itchy, reddened and swollen skin. |
| Zinc | Zinc is a mineral and can be found in topical treatments that are applied directly to the skin and oral supplements. | Zinc is an anti-inflammatory and can reduce the swelling and redness caused by acne and reduce oil production. | Orally-nausea, vomiting and diarrhoea. Topically- burning, itching, stinging and skin irritation. |
| Niacinamide | Niacinamide is vitamin B3, also known as nicotinamide and can be found in topical treatments that are applied directly to the skin and oral supplements. | Niacinamide is an anti-inflammatory and can reduce the swelling and redness caused by acne and reduce oil production. In addition, it regulates skin tone and can help to fade the red, purple and brown marks that acne can leave on the skin. | Orally- skin flushing, nausea and diarrhoea. Topically- skin irritation. |
| Retinols | Retinols are derived from vitamin A and are often labelled in products as retinaldehyde or retinyl palmitate and are not the same as retinoids. Retinols in topical treatments, are often available as creams and gels in 0.1% to 1% concentrations. | Retinols promote the growth of new skin cells whilst breaking down dead skin cells and other debris that may be trapped in the hair follicle. They also work to regulate the amount of keratin being produced by then skin and prevent dead skin cells from sticking together and forming acne-causing blockages. In addition, retinols can regulate skin tone and reduce the red, purple and brown skin markings. | Topically- irritation, redness, dryness and peeling. They can also make the skin more sensitive to the sun, so they should be applied at night and a non-oily sunscreen used during the day. |
| Alpha-hydroxy acids | Alpha-hydroxy acids, such as glycolic and lactobionic acid, are chemical exfoliators. | Alpha-hydroxy acids work by penetrating the skin and breaking-up acne-causing blockages. They can be effective at reducing pigmentation. | Topically- irritation, redness, and burning. They can also make the skin more sensitive to the sun, so they should be applied at night and a non-oily sunscreen used during the day. |
| Vitamin A | Vitamin A is available as oral tablets and is generally not as effective as other vitamin A based treatments, such as retinols and retinoids. | Vitamin A can cause skin irritation, dryness and peeling, and make the skin more sensitive to the sun. Further side effects of vitamin A include vomiting, diarrhoea, liver complications and hair loss. | Vitamin A encourages the growth of new skin cells and breaks down dead skin cells. It also works by regulating the amount of keratin being produced and prevents dead skin cells from sticking together and forming acne-causing blockages. In addition, it can regulate skin tone and reduce the red, purple and brown skin markings and reduce oil production. |
References
Related Article: Postnatal contraception advice reduces the risk of back-to-back pregnancies
- Lavers I. Acne vulgaris – diagnosis, management and optimising patient care. Dermatol Nurs 2014;13:16-25
- Layton A, Mawson R. The psychological impact of acne should not be underestimated. Buckinghamshire;Guidelines in Practice:2012
- Cunliffe T. Acne: acne vulgaris. Hertfordshire;Primary Care Dermatology Society:2018
- Lawton S. Latest treatments for acne. London;Nursing in Practice:2017
- Acne Support. Treatment. London;British Dermatology Association:2018
Resources
- Primary Care Dermatology Society. Acne: acne vulgaris pcds.org.uk/clinical-guidance/acne-vulgaris
- Acne Support acnesupport.org.uk
- British Association of Dermatologists. Patient information leaflet – acne bad.org.uk/shared/get-file.ashx?id=65&itemtype=document
- NICE. CKS: acne vulgaris cks.nice.org.uk/acne-vulgaris#!topicsummary
- DermNet New Zealand dermnetnz.org/topics/acne-vulgaris
- Primary Care Dermatology Society. Acne – primary care treatment pathway pcds.org.uk/ee/images/uploads/general/Acne_Treatment_2015-web.pdf
- Electronic Medicines Compendium medicines.org.uk/emc/
- British Journal of Dermatology. Use of isotretinoin in acne bad.org.uk/shared/get-file.ashx?id=50&itemtype=document

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom


Effective management of acne requires support and should include practical realistic advice about caring for the skin.



