Measles: What nurses in primary care need to know
GP Dr Toni Hazell outlines why we are seeing a resurgence in measles, the key clinical signs and symptoms to look out for, and how to deal with a suspected case
Anyone who keeps up to date with the news is probably feeling uneasy at the moment, with reports of spiralling cases of measles – a highly infectious viral infection, with the potential to cause serious illness and death.
Measles is possibly the most infectious virus of all time. During the Covid-19 pandemic we all became a bit obsessed with the ‘R number’ – the number of people that would be infected by a single person with Covid-19. In that case R numbers were generally in the low single figures. In contrast, the R number for measles is 12–18,1 so a single infected person will spread it widely.
So why should we be particularly worried about measles? It’s an infection that many of us have never seen, as there are few healthcare professionals working now who were also practising in the 1960s, when 80% of the population had measles in childhood. Infections and deaths fell after the introduction of vaccination in 1968, and the UK had measles elimination status in 2016/17, meaning that the condition was no longer endemic. Unfortunately, that didn’t last long, with transmission recurring in 2018.2
In 2022, there were 54 cases of measles in England and Wales – by 2023 this had risen to 209, with over half of those being seen in London.3 Worryingly, in the 14 weeks between 1 October 2023 and 18 January 2024, there have been 216 confirmed cases and 103 probable ones in the West Midlands alone, with the UK Health Security Agency (UKHSA) declaring a national incident.4
It will come as no surprise to GPs and nurses that the rising incidence of measles is intrinsically linked to vaccine scepticism. Many will remember the discredited theories of Andrew Wakefield, the scientist with significant financial conflicts of interest who linked autism to the MMR vaccine in 1998,5 and the UK has never met the World Health Organization (WHO) target of 95% coverage with two doses of the MMR.
As of September 2023, MMR uptake in England stands at 89.7% for the first vaccine and 85.5% for the second, with some London boroughs having uptake levels as low as 60%,7 despite tailored programmes which attempt to increase confidence in communities with a history of vaccine scepticism.8
Serious complications of measles
It is important to understand that measles isn’t just a harmless childhood rite of passage. Prior to vaccination there were around 100 deaths from measles each year in the UK2 and it remains an infection which carries a serious risk of complications, as listed in the box below.
Most of the complications will be seen at the time of the initial infection, but subacute sclerosing panencephalitis may present around seven years later, when an individual who previously had measles develops seizures and a worsening of neurological function. It is always fatal.
Our attempts to make the public understand how risky measles is will probably never be as articulate as the words of Roald Dahl, speaking after the death of his daughter Olivia:9
‘Olivia, my eldest daughter, caught measles when she was seven years old. As the illness took its usual course I can remember reading to her often in bed and not feeling particularly alarmed about it. Then one morning, when she was well on the road to recovery, I was sitting on her bed showing her how to fashion little animals out of coloured pipe-cleaners, and when it came to her turn to make one herself, I noticed that her fingers and her mind were not working together and she couldn’t do anything. “Are you feeling all right?” I asked her. “I feel all sleepy,” she said. In an hour, she was unconscious. In twelve hours she was dead.’
Complications of measles:2
Diarrhoea (8%)
Related Article: GPNs told to wear PPE when dealing with suspected measles
Otitis media (7–9%)
Pneumonitis
Tracheobronchitis
Pneumonia (1–6%)
Convulsions (0.5%)
Encephalitis (0.1%)
Subacute sclerosing panencephalitis (0.004%)
Keratoconjunctivitis
Clinical features – what to look for
The clinical course2 of measles starts with symptoms that are common – fever, malaise, cough, conjunctivitis and coryzal symptoms. The person is infective during this prodrome, but the underlying cause is often not recognised until the rash appears at around day 2-4.
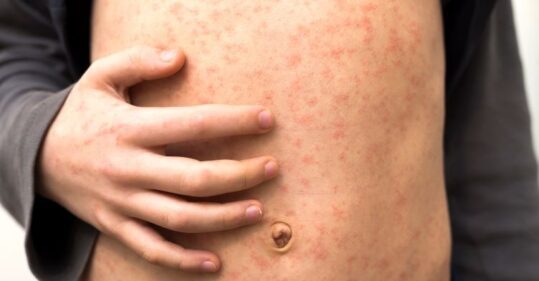
Key features include the fact that the rash appears first on the face and behind the ears, spreading to the rest of the body (trunk and limbs first, then hands and feet) over a few days, and fading after 5-7 days. It is maculopapular and becomes confluent over time.
Some patients will have Koplik spots – red spots on the buccal mucosa, with white centres, which appear around the same time as the rash. These are pathognomonic but are not always seen. The differential diagnosis includes many conditions which present with a fever and rash, including parvovirus, scarlet fever, rubella, roseola infantum, infectious mononucleosis, Kawasaki’s disease and early meningitis. Tropical diseases might also be considered in those with a recent travel history; in those without an obvious prodrome, but with a recently started new medication, it is possible that the rash of a drug reaction might look similar.
Controlling transmission
Measles is a notifiable disease,10 which means that doctors have a statutory duty to report any suspected cases. Involving our local public health team is also important to confirm the diagnosis, as it is usually them who arrange for oral fluid test kits to be sent out to the patient.11 In some areas the notification form may directly prompt the arrangement of such swabs – if you don’t know how to arrange this in the area where you work, it would be useful to find this information and cascade it to your whole practice team, before you need it.
Related Article: Labour promises ‘healthiest ever’ generation of children
Think about how you would manage a patient in whom a phone conversation raised the suspicion of measles, and you felt that they needed to be seen – how could that be arranged so that they didn’t sit in the waiting room next to your elderly or immunocompromised patients? Could they come in via a side or back door, directly into a clinical room, and out via the same direct route?
What treatment and support general practice can offer
There is no specific treatment for measles, so care is usually supportive, although NICE advises seeking advice from public health or the patient’s consultant, if a person has a measles-like rash and is pregnant, immunocompromised, or aged under one.2 Those with suspected measles should ideally stay home until no longer infective and children should stay away from school or nursery for at least four days from the first appearance of the rash.12,13
Vulnerable groups include all unvaccinated adults (who are more likely to have complications than children), those who are immunocompromised and anyone with a chronic illness. Unvaccinated pregnant women should also avoid contact with measles, as it is associated with premature labour, intrauterine death, miscarriage and stillbirth, as well as with increased maternal mortality.2 While those who are vaccinated can occasionally contract measles, this is rare, infectivity is lower and symptoms are usually mild.2 Written advice should be given so that the patient or parent of a child with suspected measles knows what to look for in terms of potential complications.14
Encouraging and supporting MMR uptake
General practice plays a key role in promoting vaccination and trying to fight against the rising tide of the anti-vaccine lobby. We can categorically say that the MMR vaccine doesn’t cause autism, and the following facts from The Green Book may be useful when having conversations with patients.15
- Children who have had the MMR don’t have an increased risk of autism compared to unvaccinated children.
- Symptoms of autism aren’t clustered around the period after the vaccination.
- When Japan discontinued the MMR in 1993, the incidence of autism continued to rise.
- There is no correlation between autism rates and vaccine coverage.
- No vaccine virus can be detected in children with autism.
Those who have religious concerns about porcine gelatine in the MMR vaccine could be signposted to information relevant to their particular religion; if the patient remains concerned, they can be offered a different brand which does not contain porcine gelatine.18
The ‘Wakefield generation’ who missed out on vaccination in 1998 and the subsequent years are now in their mid-20s – a practice could usefully consider reaching out to patients of that age group who are unvaccinated, and who can now give their own consent, rather than relying on their parents to do it for them. This can be done as part of the national catch-up campaign on MMR under which practices are required to support the national call and recall campaign and offer opportunistic catch-up vaccinations in those aged six up to 25 years old. Other quality improvement projects might include auditing the numbers of unvaccinated children, and checking if a healthcare professional has spoken to the parents to try and allay their concerns, as well as liaising with community leaders, if you have any particular groups in your practice area with specific concerns.
Dr Toni Hazell is a GP in north London
This article was initially published by our sister publication Pulse
References
- Guerra F, Bolotin S, Lim G et al. The basic reproduction number (R0) of measles: a systematic review. Lancet Infect Dis 2017 Dec;17(12):e420-e428
- NICE CKS Topics: Measles October 2022
- Iacobucci G. Measles: Warning given over low MMR uptake after cases rise to 200 in West Midlands. BMJ2024;384:q113
- UKHSA. Measles outbreak could spread warns UKHSA chief executive. January 2024
- Medscape. Top tips: vaccination myth-busting. December 2019
- UKHSA. Quarterly vaccination coverage statistics for children aged up to 5 years in the UK (COVER programme): July to September 2022. 2023
- Evening Standard. Which London boroughs have the lowest measles vaccination rates? Capital’s least protected areas revealed. January 2024
- Public Health England. Tailoring immunisation programmes: Charedi community, north London. 2018
- Roalddahlfans.com. Measles: a dangerous illness
- UKHSA. Notifiable diseases and causative organisms: how to report. January 2024. https://www.gov.uk/guidance/notifiable-diseases-and-causative-organisms-how-to-report
- UKHSA. Measles: symptoms, diagnosis, complications and treatment (factsheet). 2014
- UK Government. Department for Education. What to do if you think your child has measles and when to keep them off school. January 2024
- UKHSA. How long should you you’re your child off school – checklist poster. 2022
- NHS UK. Conditions: measles. 2022
- UKHSA. Measles: the Green book, Chapter 21. 2019
- UKHSA. Consent: The Green book, Chapter 2. 2021
- Medical Protection Society. Parental responsibility. 2020
- UKHSA. Patient leaflet: Vaccines and porcine gelatine. 2022
Local public health teams
England: Find your local health protection team here
Related Article: ‘Urgent’ measles action required as UKHSA declares ‘national incident’
Northern Ireland: Phone 0300 555 0114 or contact the Public Health Agency here
Scotland: Find your local health protection team here
Wales: Phone 0300 00 300 32 or go to the Public Health Wales information page

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom

