Ten top tips for nurses on Lyme disease
With the arrival of spring, ticks that spread Lyme disease may be getting more active – just as more people are getting out into our parks and countryside. Here GP Dr Rachael Llewelyn and nurse Julia Knight offer their ten top tips for practice nurses to spot and treat Lyme disease promptly
- Lyme disease can be contracted anywhere in the UK
The infection is spread by ticks that are infected with Borrelia bacteria. The incidence of Lyme disease is increasing and it is the most common tick-borne disease in the Northern Hemisphere. Infected ticks can be found throughout the UK – some areas are known to be higher risk, including the Highlands of Scotland, South and Southwest England and parts of East Anglia, but infection can occur in any area. Ticks are mainly found in grassy areas and woodlands but have also been found in urban parks and gardens.
- People pick up ticks from grass
Ticks look for food by ‘questing’ – waiting on a blade of grass for a host to brush by, then transferring onto the host and finding somewhere to embed themselves. People who spend a lot of time outdoors in the countryside, either for leisure (walkers, campers) or through their occupation (foresters, gardeners, vets) are at higher risk of tick bites, but keep in mind that anybody can sustain a tick bite.
Ticks are usually most active from early spring to late autumn. However, with our changing climate and the UK now having milder winters with more rainfall, ticks now appear to be active in some areas throughout the year.
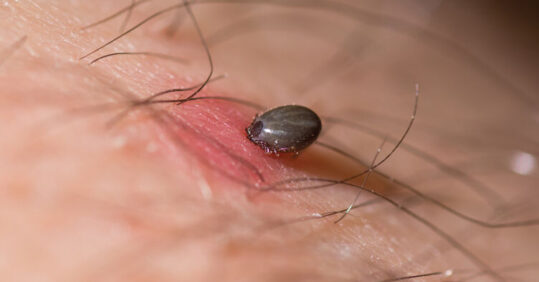
- Ticks like to embed in a warm, concealed place
Ticks tend to embed in a warm, unexposed part of the body like the groin, armpit, waistband or hair line. Once embedded, they will feed for a few days and eventually fall off. Ticks can feed for between three and six days. Often people don’t realise they have been bitten. If they do, then the tick should only be removed using a special tool – as explained in point 4.
Related Article: NHSE confirms dates and eligibility for autumn Covid and flu jabs
- Always remove ticks with a tick-removing tool
If a patient presents with an embedded tick, it must be removed with a special tick removal tool (see Image 1, below) or fine tipped tweezers only. Never stress the tick by covering it with something such as Vaseline as this can actually increase the risk of transmission – a stressed tick may regurgitate the contents of its stomach into the host’s bloodstream.

If a tick tool is available, slide the fork-like part of the tool underneath the tick, twist the tool (to loosen the grip of the tick) and pull upwards. There should be instructions with the tool. If using fine tipped tweezers, grasp the tick as close to the skin as possible and pull straight upwards. Clean the area with an antiseptic wipe and provide the patient with advice about what symptoms to look out for over the next few weeks. If the tick is not removed cleanly and the mouthparts remain embedded, the body will dispel them like any other foreign body, but the patient should be advised to observe for any signs of localised infection that might need treatment. Retained mouthparts do not increase the risk of contracting Lyme disease.
Preventative treatment after a tick bite is not usually recommended by the NHS, but the RCGP Lyme disease toolkit suggests this can sometimes be considered for certain high-risk cases.
It is estimated that only about 10% of ticks carry the bacteria that causes Lyme disease, which can be reassuring when a person seeks advice after a tick bite.
- Lyme disease can be diagnosed by a distinctive erythema migrans rash
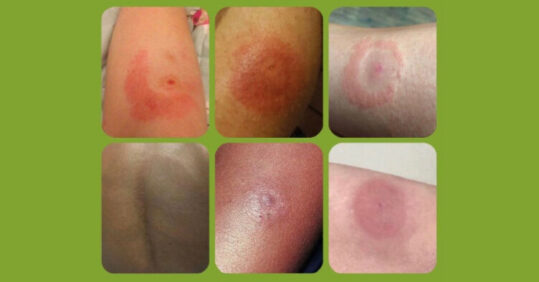
The most obvious sign of Lyme disease is an erythema migrans (EM) rash, sometimes referred to as a ‘bullseye’ rash. However, bear in mind that about 30% of people infected with Lyme disease do not develop a rash (see point 7).
As well as the typical bullseye presentation, the rash can have solid or bruise like appearance; it can also present very differently on darker skin tones and be harder to spot (see Figure 1, below). The behaviour of the rash is very important when considering diagnosis. Unlike other insect bites, it is slow to appear (from three days after a bite, up to three months), is generally not itchy or painful and gradually spreads outwards. As the name indicates, it is this gradual spreading that is often the tell-tale sign of an EM rash. In some cases, EM rashes can become huge. Any redness, itchiness or swelling immediately after a bite is likely to be a histamine reaction rather than EM.
- Treatment should be started promptly with antibiotics
If an EM rash is identified, treatment with antibiotics should begin straight away. There is no need for a blood test as the EM rash is diagnostic for Lyme disease. Antibiotics should be prescribed according to the NICE guideline recommendations for treating Lyme disease. It is important to note that antibiotic dosages for children with Lyme disease are much higher than for other infections and are based on the child’s age and weight. The NICE guidelines should always be consulted if the clinician is not familiar with prescribing for Lyme disease.
- Lyme disease can also cause flu-like symptoms
As explained above, Lyme disease does not always present with a rash. Other symptoms to look out for include flu-like symptoms, headache, neck ache, sore muscles and joint pain (particularly if the pain is migratory in nature), fatigue, malaise, brain fog, paraesthesia and feeling generally very unwell. Good history taking is essential, especially if the person doesn’t recall a tick bite. Travel history and occupation may give you a hint, but many people sustain a bite doing nothing outside of their usual routine such as walking their dog.
Related Article: Gypsy, Roma and Traveller healthcare: How can primary care serve this group?
- Laboratory tests can be used if diagnosis is uncertain
If Lyme disease is suspected but there is no EM rash present, serology testing should be carried out. Testing for Lyme disease in the UK is a two-tier system. The first tier is an Elisa test. If this returns a positive or equivocal result it should be followed by the second tier of testing, an immunoblot, to rule out any cross-reactions from the initial test.
The immunoblot is carried out by the National Reference laboratories at Porton Down in England and Wales, and Raigmore in Scotland. Both are antibody tests, and it is important to remember that the immune system can take some time to make antibodies to the bacteria that causes Lyme disease, possibly up to four weeks or even longer. Therefore, testing straight after a bite is likely to return a negative result even if the person has been infected. If a test is carried out during this early window, it should be repeated. The NICE guidelines recommend clinicians should consider starting treatment while waiting for the results of testing if there is high clinical suspicion of Lyme disease, and that they should be aware that testing can produce both false positive and false negative results.
- Early recognition is vital for complete recovery
Early recognition and treatment of Lyme disease is essential for a complete resolution of symptoms. Many people who contract Lyme disease have no recollection of being bitten by a tick; at certain times in the tick life cycle, ticks can be as small as a poppy seed and are easily missed. If there is no EM rash present and a patient does not recall a tick bite, it is essential that diagnosis is based on a combination of careful history, clinical presentation and if necessary, serology testing. Lyme disease should not be ruled out based on a negative testing alone due to the unreliability of testing.
- Late diagnosis can lead to long-term complications
Late diagnosis or misdiagnosis can lead to long-term debilitating symptoms, so it is important for nurses to be aware of the complexities of the disease and to be able to recognise it. Disseminated Lyme disease can cause damage to the nervous system, heart and joints. Even after treatment people may take several months to recover and some may be left with residual symptoms.
Prompt diagnosis and treatment are essential to help mitigate this.
Related Article: Public urged to see practice nurse before travelling amid high enteric fever cases
Dr Rachael Llewelyn is a GP and contributor to the RCGP Lyme disease Spotlight Project and Julia Knight is a registered nurse and Lyme Disease UK outreach manager
Useful reading
- NICE NG95. Lyme disease. 2018. Available at: nice.org.uk/guidance/ng95
- RCGP e-learning: Lyme disease toolkit. https://elearning.rcgp.org.uk/mod/book/view.php?id=12535
- Lyme disease UK. Further resources for healthcare professionals https://lymediseaseuk.com/hcp-further-resources/

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom




