Understanding shingles and the extended vaccination campaign
Autumn saw the start of an NHS vaccination campaign targeting almost a million people with the Shingrix vaccine. Here, nurse consultant Linda Nazarko explains the background to the programme, and advises on diagnosing and treating shingles and its associated complications
What is shingles?
Shingles is a painful blistering rash caused by reactivation of varicella zoster virus, the chickenpox virus. It is correctly known as herpes zoster.1
Almost everyone is infected with the chickenpox virus during childhood.2 On recovery, the virus remains dormant in the spinal nerves for life. It can reactivate when the immune system is compromised, so ageing increases the risk of developing shingles, because the immune system becomes less effective with age.3 Each year around 50,000 people over 70 in England and Wales are affected4, and more than half of adults who have had chickenpox will develop shingles by the age of 85.5
Diseases like HIV and lymphoma, and medications such as steroids depress the immune system and increase the risk of shingles, as do statins.6,7 Older people with severe depression are more likely to develop shingles as depression also affects the immune system.8
The prevalence of shingles has prompted NHS England to extend the vaccination programme to cover almost a million people over the next decade.
Clinical features of shingles
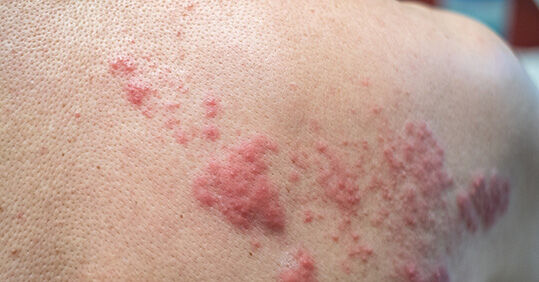
The person may feel unwell, with a headache, generalised aching and a mild temperature before the rash is seen. The rash normally appears along a single dermatome – an area of skin supplied by a single spinal nerve. At first, the rash is red with tiny blisters or vesicles that can be intensely itchy. In the next 72 hours, it extends along the dermatome and the vesicles become larger as they fill with fluid. After three to five days, these burst and begin to dry and crust, normally healing within 10-14 days.9
However, the rash can leave pigmentation – this varies but is noticeably different to the person’s normal skin colour.9 It often settles quickly, but can persist for 12 months or longer. It can be treated topically with vitamin C, retinoids, azelaic acid or short-term topical steroids.
Treatment
Shingles is painful and distressing. Treatment aims to reduce the severity of the attack, ease pain and discomfort, accelerate healing and protect others from potential infection. Treatment is normally with oral antivirals such as acyclovir, famciclovir and valaciclovir. If infection is very severe or the person is especially vulnerable, these may be given intravenously.
Related Article: New ‘life-extending’ drug for ovarian cancer added to NHS
Antiviral treatment reduces rash, pain and complications such as postherpetic neuralgia (PHN).10 It prevents the virus multiplying and may limit the extent of the attack. Treatment should begin at diagnosis, as antivirals work best within 72 hours of rash onset.11
If there are delays in diagnosis, antivirals will still be beneficial if the person has severe pain or the rash is continuing to progress.12,13
Corticosteroids such as prednisolone may be prescribed in severe infections to reduce pain and inflammation and increase the rate of healing. Evidence supports their ability to reduce acute pain but there is little evidence that they improve wound healing or prevent PHN.14,15
NICE recommends consideration of oral corticosteroids in combination with antiviral medication if pain is severe, in the first two weeks after rash onset in immunocompetent adults with localised shingles.16
Pain can be treated with paracetamol alone or in combination with codeine or a nonsteroidal anti-inflammatory drug (such as ibuprofen). It is important that these are taken regularly.14 Itching can be treated by antihistamines such as chlorpheniramine (Piriton).
Infection risks
Vesicles contain the herpes varicella zoster virus and contact with vesicle liquid could potentially cause chickenpox infection in a person who has not had it earlier in life. The risk is very low since most people have immunity through childhood exposure to chickenpox.
A person with shingles should be advised to avoid contact with anyone who has not had chickenpox, particularly pregnant women and immunocompromised people, as well as babies who are less than a month old.
In the family home, the bedlinen, clothing and towels used by the person with shingles should be laundered separately until the rash has dried up. Any weeping vesicles should be covered with a dressing to avoid the virus coming in contact with people vulnerable to chickenpox.
Primary care staff should follow their local infection-control policy and use protective equipment if there is a risk of contact with blood and body fluids.
Complications
While people normally recover from shingles without any additional issues, there are a number of potentially serious complications (Table 1).17 The most common are PHN and secondary infection. A third of patients aged 80 and older develop PHN, as do a fifth of over-50s.18 Pain is usually unilateral and can be shooting, stabbing or burning. Treatment is with topical or oral medication.19
Table 1: Complications of shingles 17
Type of complication
Details
Neurological
Neuropathic pain. Cranial and peripheral nerve palsies (excluding Ramsay Hunt syndrome), encephalitis, transverse myelitis, meningitis, Guillain-Barré syndrome, stroke
Ophthalmic
Keratitis, conjunctivitis, iritis, blepharitis, retinitis, optic neuritis, orbital myositis, scleritis, glaucoma, vision loss or blindness, nonspecific eye infections
Cutaneous
Secondary bacterial skin infection (cellulitis, necrotising fasciitis and erysipelas)
Visceral and systemic
Pneumonia, hepatitis, pancreatitis, sepsis, pulmonary embolism, osteomyelitis, pleuritis, peritonitis, myocardial infarction, myositis, myocarditis, pericarditis and endocarditis
Zoster-specific complications
Ramsay Hunt syndrome, varicella zoster virus dissemination
NICE recommends simple analgesia such as paracetamol, but codeine may be added if required.20 Medications to treat neuropathic pain include amitriptyline (10-20mg)21 and duloxetine.22 The anticonvulsants gabapentin and pregabalin can be used22 but can cause drowsiness and increase risk of falls, especially in frail older people. Capsaicin, the component of chilli peppers that causes burning, can be applied in cream form.23 Skin patches with 5 or 8 per cent lidocaine can be applied to the painful area for around 12 hours in a 24-hour period.24 The 5 per cent patch has fewer side-effects, is better tolerated and works faster.
Related Article: Reframing eating disorder recognition in primary care
Secondary bacterial infection can occur, so good hygiene is important. Affected skin can be washed with clear water and patted dry gently. The person should wear soft, light clothing that is changed at least daily.
If skin becomes hot, itchy and uncomfortable topical therapy such as calamine lotion may help. Gauze soaked in Burow’s solution (5 per cent aluminium acetate) can cool and soothe the skin and is also thought to have antibacterial properties that can cut the risk of infection.
If the rash is weeping, then non-adherent dressings should be used and changed as necessary. Antibiotic therapy may be required to treat any secondary infection.
Around 10 per cent of people with shingles develop ophthalmic complications.25 A small number who develop eye or neurological complications may not have had a rash.26 People who have neurological or eye symptoms are at risk of ophthalmic complications and should be referred for appropriate specialist advice.
Immunisation programme
The NHS shingles vaccination programme began in 2013. The number of people being vaccinated is rising, with around 44% of 71-year-olds and 82% of 79-year-olds now treated under the programme.27 Vaccination is reported to have averted 40,500 GP consultations and 1,840 hospitalisations in England over a five-year period.28
Two vaccines were initially introduced: Zostavax MSD, a live attenuated virus given to most eligible people, and Shingrix GSK (a recombinant sub-unit vaccine), given to the immunocompromised (see Table 2).29,30
Table 2: Details of shingles vaccines29,30
Vaccine
Characteristics
Dosage and cost
Indications
Zostavax (MSD)
Live attenuated virus
Single dose, 0.65ml
£99.96Prevention of herpes zoster and postherpetic neuralgia in adults
Shingrix (GSK)
Recombinant
Two doses of 0.5ml each,
two months apart
£160 per dosePrevention of herpes zoster and postherpetic neuralgia in adults >50 years
Adults >18 years of age at increased risk of herpes zoster
From September, Shingrix is given routinely to all eligible people via two doses, two months apart.31 The Shingrix vaccine is 97.2% effective, a significant improvement on 51% for Zostavax.32 The plan is to immunise all over-60s across a 10-year period. The first phase this year will target those turning 70 and 65, and anyone over 50 who is immunocompromised, in addition to those aged 70-80. The changes mean almost a million people in England will fall into eligible cohorts by 2033.33
Related Article: Sharp rise in diabetes cases prompts call for better postnatal support
Preparing for vaccinations
Primary care staff can identify those eligible and ensure they are aware they can get the vaccine, which can be given at the same time as flu vaccination. If more than one vaccine is given at the same appointment, they should preferably be in different arms. If given in the same limb, they should be given at least 2.5cm apart.
Linda Nazarko is a nurse consultant in physical health care at West London NHS Trust
References
- Oakley A (2015). Shingles (Herpes Zoster). DermNet NZ, New Zealand. Link
- Walker J et al. (2017) Trends in the burden of varicella in UK general practice. Epidemiol Infect. 145(13):2678-2682.
- Pawelec G. (2102) Hallmarks of human “immunosenescence”: adaptation or dysregulation? Immun Ageing. 25;9:15. Link
- The Green Book. Chapter 28a: Singles (herpes zoster). UK Health Security Agency, July 2023. Link
- Nagel M et al. (2020) Central nervous system infections produced by varicella zoster virus. Curr Opin Infect Dis. 33;3:273-8. Link.
- Antoniou Tet al. (2014) Statins and the Risk of Herpes Zoster: A Population-Based Cohort Study. Clin Infect Dis: 58;3:350-6. Link
- Chung SD et al. (2014) Herpes zoster is associated with prior statin use: a population-based case-control study. PLoS One. 24;9(10):e111268. Link
- Irwin M et al. (2011) Major depressive disorder and immunity to varicella-zoster virus in the elderly. Brain Behav Immun. 25:4:759-766. Link
- National Institute for Health and Care Excellence. Shingles. Clinical Knowledge Survey. 2023. Link
- Lilie H and Wassilew S (2003). The role of antivirals in the management of neuropathic pain in the older patient with herpes zoster. Drugs & Aging 20:8:561-570.
- Wood M et al. (1998) Treatment of acute herpes zoster: effect of early (< 48 h) versus late (48–72h) therapy with acyclovir and valaciclovir on prolonged pain. J Infect Dis 178 Suppl 1: S81-S84
- Johnson R and Whitely R (Eds). (2006) International Herpes Management Forum. Combating varicella zoster virus-related diseases. Herpes 13 Suppl 1: 1-41
- Dworkin R et al. (2007) Recommendations for the management of herpes zoster. Clin Infect Dis 44 Suppl 1: S1-S26. Link
- Han Y et al. (2013) Corticosteroids for preventing postherpetic neuralgia. Cochrane Database Syst Rev. 28;3:CD005582. Link
- Opstelten W et al. (2008) Treatment of herpes zoster. Can Fam Physician 54:3:373-377. Link
- NICE. Shingles: Corticosteroids. CKS, London 2016. Link
- Forbes, H et al. (2021) Incidence of acute complications of herpes zoster among immunocompetent adults in England: a matched cohort study using routine health data. Br J Dermatol 184: 1077-1084. Link 1084.
- Yawn B and Gilden D.(2013) The global epidemiology of herpes zoster. Neurology 81(10):928-30. Link
- Nalamachu S and Morley-Forster P. (2012) Diagnosing and managing postherpetic neuralgia. Drugs & Aging. 29:11:863-9.
- NICE CKS. Post-herpetic neuralgia. NICE, London 2022. Link
- Moore R et al. (2015) Amitriptyline for neuropathic pain in adults. Cochrane Database Syst Rev. 6;2015(7):CD008242. Link
- Saarto T and Wiffen P. (2007) Antidepressants for neuropathic pain. Cochrane Database Syst Rev. 17;(4):CD005454. Link
- Derry, S et al. (2017) Topical capsaicin (high concentration) for chronic neuropathic pain in adults. Cochrane database Syst Rev 1(1), CD007393. Link
- Christo P et al. (2007) Post-herpetic neuralgia in Older Adults: Evidence-based Approaches to Clinical Management. Drugs & Aging 24:1: 1-19
- Opstelten W et al. (2005) Managing ophthalmic herpes zoster in primary care. BMJ 331(7509): 147–151. Link
- Nagel M and Gilden D. (2013) Complications of Varicella Zoster Virus Reactivation. Curr Treat Options Neurol. 15(4): 439–453. Link
- NHS England (2023). Research and analysis. Shingles vaccine coverage (England): report for quarter 1 of the financial year 2022 to 2023. Link
- Andrews N et al. (2020) Impact of the herpes zoster vaccination programme on hospitalized and general practice consulted herpes zoster in the five years after its introduction in England: a population-based study. BMJ Open 10:e037458. Link
- BNF Herpes-zoster vaccine (live) Medicinal forms. 2023. Link
- BNF Herpes-zoster vaccine (recombinant, adjuvanted) Medicinal forms. 2023. Link
- NHS England. Correspondence: Introduction of Shingrix® vaccine for the whole programme and expansion of eligible cohorts letter. July 2023. Link
- Anderson LA (2022). Shingrix vs Zostavax – What’s the difference between them? Drugs.com. Link
- NHS England (2023b) NHS shingles vaccine will be offered to almost one million more people. July 2023. Link

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom