Asking about periods and pregnancy could reduce a woman’s risk of cardiovascular disease
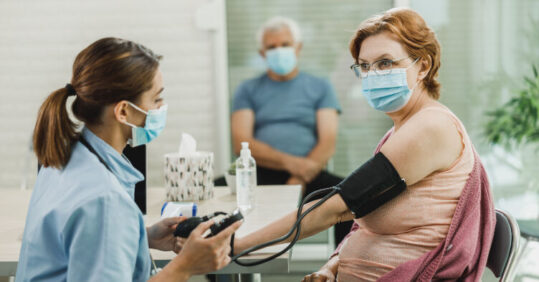
Reproductive factors such as a high number of live births and starting periods at a young age can increase a woman’s risk of cardiovascular disease, according to a new study.
Related Article: Diagnosis Connect service will link people to advice from charities
The findings published in the Journal of the American Heart Association highlight the need for clinicians to monitor sex-specific risk factors for heart disease and intervene where needed.
Women are often mischaracterised as being at low risk for cardiovascular disease. However, heart problems are responsible for twice as many deaths in women as breast cancer in the UK each year. According to the British Heart Foundation, there are more than 800 000 women in the UK living with cardiovascular disease but even when they are diagnosed, it is found that women tend to receive less targeted treatment than men.
The researchers undertook a genome-wide study (GWAS), which compares the genomes of different people to find genetic markers associated with a particular disease. In this case, they looked at genetic data from over 100 000 women linked to a women’s age at first birth, their number of live births, their age at their first period, and their age at menopause and their associated risk of cardiovascular disease. Statistical techniques were applied to the data to remove the influence of factors such as diet, socioeconomic status and exercise levels.
The analysis showed that an earlier first birth, a higher number of live births, and an earlier first menstrual cycle were associated with heart disease in women. There was no link established between the age of menopause and cardiovascular disease.
Related Article: CVD prevention must be national health priority, says report
Dr Maddalena Ardissino, lead author of the study, said that even though the study shows a clear link between reproductive factors and cardiovascular disease, women should not worry if they’ve had their period at a young age or if they had an early first birth.
She explained: ‘Our research shows that the additional risk of cardiovascular disease can be minimised if traditional risk factors like BMI and blood pressure are well-controlled.’
Many of the previous studies on cardiovascular disease have focused on men, but the team’s new findings show clear sex-specific factors that influence the risk for women. A significant part of the increased risk from early menstruation resulted from this factor being associated with a higher body mass index (BMI). The researchers suggest that lowering a person’s BMI could help this.
Related Article: Prescribing in England to be led by a single national formulary
Dr Fu Siong Ng, from Imperial College, said: ‘While we cannot say exactly how much these factors increase the risk of cardiovascular disease, our study shows that reproductive history is important, and it points towards a causal impact. We need to understand more about these factors to make sure that women get the best possible care.’

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom




