Management of pressure ulcers
Pressure ulcers present a very real problem in almost all healthcare settings, so it is important that nurses are equipped to prevent and identify the condition.
Pressure ulcers remain a serious and potentially life-threatening problem across all age groups from the very young to the very old and across all medical specialties and care settings. Overall, up to £4 billion (4% of NHS spending1) is spent treating pressure ulcers and related conditions annually with individual costs of treating the most severe cases ranging from £11,000 to £40,000. The cost of interventions to prevent pressure ulcers is inestimable.2 With an estimated 20% of hospitalised patients (equating to around 20,000 hospitalised patients at any one time) developing pressure ulcers2 and many more in the community and in care homes, estimated to be around 30,000,3 the time is ripe to direct efforts to eradicate this problem.The vast majority of pressure ulcers are avoidableand therefore the associated health service and independent sector financial costs and far-reaching negative impact on individuals could also be avoided.
The National Patient Safety Agency (NPSA) (2010)3 believes the solution to this problem to be simple and summarises it as: observing patients’ skin, changing the position of patients at regular intervals as well as checking for a moisture-free environment, and monitoring their nutritional statuses. The focus for the NPSA national quality and productivity agenda aims to reduce harm from pressure ulcers as a matter of urgency. All efforts should be focused not only on following this advice but also increasing and rationalising carers’ knowledge and experience in pressure ulcer prevention.
Pressure ulcers
A pressure ulcer is defined as “localised injury to the skin and/or underlying tissue usually over a bony prominence, as a result of pressure, or pressure in combination with shear. A number of contributing or confounding factors are also associated with pressure ulcers; the significance of these factors is yet to be elucidated.”4 This definition was agreed as part of international guidelines published in an attempt to standardise and improve practice in relation to pressure ulcer prevention, assessment and management globally.
Pressure ulcers may present as discoloration of the skin to extensive insults to bone level with destruction of the skin, subcutaneous tissue and bone. Although understanding is incomplete, sustained pressure (the weight of the body pressing down on the skin) is thought to be the most significant contributing mechanical force for pressure ulceration5 due to its tissue distorting effects. Pressure, in combination with shear (when layers of skin are forced to slide) which integrates elements of frictional forces (deformation of tissues), particularly near a bony prominence is believed to cause pressure ulceration6. More recently, attention has turned to the influence of skin microclimate on tissue breakdown. Skin may be weakened and the risk for pressure ulceration increased by the presence of excessive moisture due to perspiration, urinary or faecal incontinence, wound/fistula drainage or vomit, although more research is needed.7
Pressure ulcers can develop in any area of the body,8 but particularly over the bony prominences of the sacrum, heels and ischial tuberosities depending on the position of the patient. In children and infants the damage is more likely to occur over the occiput or ears.9
Patient assessment
The first step in pressure ulcer prevention involves assessing the patient’s risk factors, which include intrinsic and extrinsic factors. The patient’s current health status, acute, chronic and terminal illness, co-morbidities such as diabetes and malnutrition, mobility status, posture (pelvic obliquity and posterior pelvic tilt), sensory impairment, level of consciousness, systemic signs of infection, nutritional status, previous pressure damage, pain status, psychological factors, social factors, continence status, medication, cognitive status, and blood flow should be included in the assessment.8
A number of risk assessment scales have been developed with the Waterlow Risk Assessment Scale used most frequently in the UK across care settings. Most organisations now have established policies for pressure ulcer prevention that require patients or clients to have a formal risk assessment carried out on admission or first contact, with the frequency of re-assessment determined by the first level nurse. Despite criticism of their accuracy, validity and reliability, the wholesale adoption of risk assessment tools as aids to pressure ulcer prevention is well established and their use provides a structured approach to assessment when combined with clinical judgement. Formally risk assessing patients should prompt appropriate interventions, useful documentation and onward referrals to, for example, dietetics, tissue viability specialists and other members of the multidisciplinary team.
Related Article: Call for regulatory guidelines as NHS adopts AI in dermatology care
Pressure ulcer assessment
On finding a pressure ulcer an initial and ongoing assessment and documentation of findings are essential to best practice in monitoring and communication of progress. The cause of the ulcer, its site/location, dimensions, presence, amount and type of exudate, local signs of infection, pain, wound appearance, the surrounding skin, evidence of undermining/tracking (sinus or fistula), odour and stage/grade or category assessed and documented. It is recommended that the commentary is supported by photographs and/or tracings calibrated with a ruler.
The pressure ulcer should be categorised (staged/graded) according to the four levels of damage as agreed by the European Pressure Ulcer Advisory Panel/National Pressure Ulcer Advisory Panel (EPUAP/NPUAP) (2009).4
Category/Stage I: Non-blanchable erythema
Intact skin with non-blanchable redness of a localized area usually over a bony prominence. Darkly pigmented skin may not have visible blanching; its colour may differ from the surrounding area. The area may be painful, firm, soft, warmer or cooler as compared to adjacent tissue. Category I may be difficult to detect in individuals with dark skin tones. May indicate ‘at risk’ persons.
Category/Stage II: Partial thickness
Loss of dermis presenting as a shallow open ulcer with a red pink wound bed, without slough. May also present as an intact or open/ruptured serum-filled or sero-sanguinous filled blister. Presents as a shiny or dry shallow ulcer without slough or bruising (which indicates deep tissue injury). This category should not be used to describe skin tears, tape burns, incontinence associated dermatitis, maceration or excoriation.
Category/Stage III: Full thickness skin loss
Subcutaneous fat may be visible but bone, tendon or muscle are not exposed. Slough may be present but does not obscure the depth of tissue loss. May include undermining and tunnelling. The depth of a Category/Stage III pressure ulcer varies by anatomical location. The bridge of the nose, ear, occiput and malleolus do not have (adipose) subcutaneous tissue and Category/Stage III ulcers can be shallow. In contrast, areas of significant adiposity can develop extremely deep Category/Stage III pressure ulcers. Bone/tendon is not visible or directly palpable.
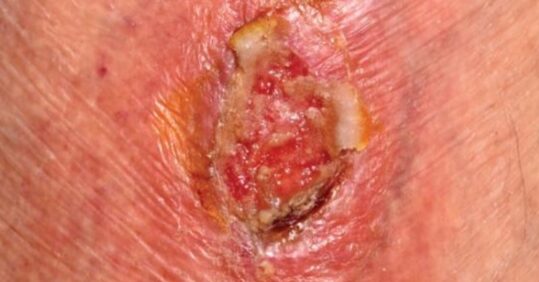
Category/Stage IV: Full thickness tissue loss
Full thickness tissue loss with exposed bone, tendon or muscle. Slough or eschar may be present. Often includes undermining and tunnelling. The depth of a Category/Stage IV pressure ulcer varies by anatomical location. The bridge of the nose, ear, occiput and malleolus do not have (adipose) subcutaneous tissue and these ulcers can be shallow. Category/Stage IV ulcers can extend into muscle and/or supporting structures (e.g., fascia, tendon or joint capsule) making osteomyelitis or osteitis likely to occur. Exposed bone/muscle is visible or directly palpable.
The EPUAP/NPUAP (2009) descriptions of categories are clear and address some of the current issues of identifying damage that is attributed to pressure, shear and friction, and not other causes such as moisture. The guidelines discuss additional categories applicable to the US system that include “full thickness tissue loss in which actual depth of the ulcer is completely obscured by slough (yellow, tan, gray, green or brown) and/or eschar (tan, brown or black) in the wound bed.” This category recognises the difficulty with accurately assessing the depth and extent of the tissue damage. A second category describes “suspected deep tissue injury” where the depth is unknown and may present as a “purple or maroon localized area of discoloured intact skin or blood-filled blister due to damage of underlying soft tissue from pressure and/or shear. The area may be preceded by tissue that is painful, firm, mushy, boggy, warmer or cooler as compared to adjacent tissue.”4 This is the type of pressure damage that can appear to rapidly progress to full thickness tissue loss.
Pressure ulcers must be differentiated from other types of skin damage such as that caused by moisture (incontinence/associated dermatitis or sweat), dressing or tape damage.
The importance of accurately staging/categorising/grading cannot be underestimated and health care professionals need to be educated in this area to be able to collate and provide reliable data for Continuous Quality Improvement Network (CQUIN) data submission.
Patient management
Once identified as at risk or with pressure ulcers, patients should be educated about their risk and encouraged and/or assisted to move themselves where possible. However, many patients will be reluctant to move due to pain or anticipation of pain, positional discomfort, the effects of sedation or analgesia, or their inability to appreciate their level of risk due to confusion or dementia. It is the nurse´s responsibility to ensure that patients are repositioned in a way that is not only therapeutic but acceptable to them.
Regular, thorough skin inspection, particularly over bony prominences, must be carried out as it is key to detecting pressure damage,10 and any redness or other marking documented and monitored. The frequency of repeat inspections will be determined by the initial findings, the individual’s level of risk for PU development and the type of healthcare setting. The finding of non-blanching erythema should alert the nurse to the possibility of pressure damage. Skin care should aim to keep skin clean using a pH balanced cleanser or emollient soap substitute, the skin dried gently and kept moisturised. A protective barrier spray or cream can be used to prevent incontinence-damaged skin from breaking down further.11
Related Article: Abdominal body fat is a higher risk for developing psoriasis
The patient assessment will direct decisions on positioning, its frequency and the choice of an appropriate support surface for both the bed and chair. Such interventions can prevent pressure damage.11 The factors that need to be considered when making choices regarding pressure reducing equipment include clinical efficacy, its impact on care procedures, ease of use and maintenance, cost and, most importantly, patient acceptance.
Adequate nutritional and fluid intake are essential for both the prevention and healing of pressure ulcers and most prevention policies and more recently, the Waterlow Risk Assessment Scale, include nutritional assessment as a key element.
Conclusion
Due to the multifactorial nature of pressure ulcers health care practitioners need educating on a wide range of patient, device and assessment-related topics, for example, pressure ulcer identification and classification, anatomy and physiology, variances and differentiation of damage from other causes, nutrition, repositioning, risk assessment skills and how to document information appropriately. Knowledge and skills should be monitored and updated annually or at least as new knowledge emerges that influences change in practice.
References
1. Clark M. Pressure Ulcers. Smith & Nephew Foundation: Hull; 2007.
2. Posnett J, Franks PJ. The costs of skin breakdown and ulceration in the UK. Smith & Nephew Foundation: Hull; 2007.
3. National Patient Safety Agency. NHS to adopt zero tolerance approach to pressure ulcers; 2010 Retrieved 1 Jan 2012 from http://www.npsa.nhs.uk/corporate/news/nhs-to-adopt-zero-tolerance-approach-to-pressure-ulcers/
4. European Pressure Ulcer Advisory Panel and National Pressure Ulcer
Advisory Panel. Prevention and treatment of pressure ulcers: quick reference guide.Washington DC: National Pressure Ulcer Advisory Panel; 2009.
5. National Institute for Health and Clinical Excellence. Pressure Ulcers: Prevention and Treatment; 2005. Retrieved 2nd Jan 2012 from http://www.nice.org.uk/nicemedia/pdf/CG029publicinfo.pdf
Related Article: CPD: Case by case – acute and emergency dermatology presentations
6. Allman RM. Pressure ulcer prevalence, incidence, risk factors, and impact. Clin Geriatr Med 1997;13:3:421-36.
7. International review. Pressure ulcer prevention: pressure, shear, friction and microclimate in context. A consensus document. London: Wounds International; 2010.
8. Rycroft-Malone J, McInnes E. Pressure ulcer risk assessment and prevention guideline: Technical Report. London: Royal College of Nursing; 2001. (Available at www.rcn.org.uk).
9. Murdoch V. Pressure care in the paediatric intensive care unit. Nurs Stand 2002;17:71-74,76.
10. International guidelines. Pressure ulcer prevention: prevalence and incidence in context. A consensus document. London: MEP Ltd; 2009. 11. Cooper P, Clark M, Bale S. Best Practice Statement: Care of the Older Person’s Skin. Wounds UK. Retrieved Jan 4th 2012 from

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom


Pressure ulcers remain a serious and potentially life-threatening problem across all age groups from the very young to the very old and across all medical specialties and care settings.