‘Smart bandages’ could reduce antibiotic use for non-healing wounds
A wirelessly-powered ‘smart bandage’ could provide drug-free wound care, helping patients with non-healing wounds, avoid infections and significantly improve their quality of life, an international team of researchers has suggested.
The first-of-its-kind bandage has been developed by researchers from the UK and France and uses ultraviolet light to kill bacteria in the wound without the need for antibiotics.
It is embedded with light-emitting diodes (LEDs), which bathe wounds in sterilising ultraviolet light, preventing the growth of bacteria and could also help to slow the rise of dangerous new strains of antibiotic-resistant bacteria known as ‘superbugs’.
Related Article: Call for regulatory guidelines as NHS adopts AI in dermatology care
In a paper published in the journal IEEE Transactions on Biomedical Circuits and Systems, the researchers outline how they built the smart bandage and demonstrated its antibacterial effectiveness. The bandage has so far been successfully tested under laboratory conditions but further trials are needed before it will be available in healthcare settings.
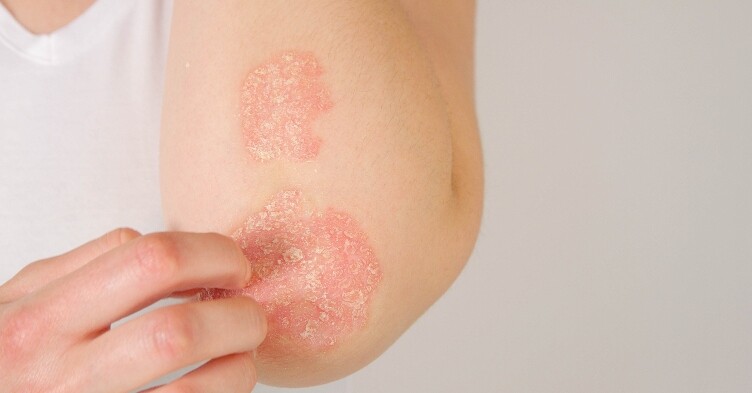
Current management of chronic non-healing wounds, which can be a side effect of some medications or arise from conditions such as cancer and diabetes, involves frequent and often painful cleaning and treatment to prevent the spread of bacteria.
UV light is already used in healthcare environments to sterilise equipment and could offer an alternative treatment to keep wounds free of bacteria. The bandage needs its own power supply to power the UV LEDs, so the researchers developed a system that provides energy without needing batteries.
The wireless power system is built around two metal coils. The first is a slim, flexible inductive coil which can be integrated into the fabric of the bandage and receives power wirelessly from a second coil connected to the electric mains. The coil in the bandage can then provide power to the LEDs whilst the coils are close to one another and until the antimicrobial treatment is complete.
Traditional batteries are bulky and inflexible and must be changed regularly, resulting in a high environmental footprint. The new wireless coil system allows the bandage to be flexible, conforming closely to the patients’ bodies and offers a sustainable way to deliver reliable treatment over several hours.
Related Article: Abdominal body fat is a higher risk for developing psoriasis
In laboratory tests, the researchers exposed samples of a strain of the gram-negative bacterium Pseudoalteromonas sp. D41, which can cause a range of severe infections in humans, to the UV light supplied by the smart bandage. The tests showed that the smart bandage could slow and stop the growth of Pseudoalteromonas sp. D41 on the surfaces of slides and effectively eradicated the bacteria within six hours.
The researchers suggest that the system could be used in medical settings and eradicate bacteria in patients’ chronic non-healing wounds.
Professor Steve Beeby, from the University of Southampton, who is a co-author of the paper, said: ‘The use of ultraviolet light to kill viruses and bacteria is well known, and this is the first work to integrate UVC emitting LEDs within a bandage and explore its efficacy.’
Related Article: CPD: Case by case – acute and emergency dermatology presentations
He added: ‘This approach could provide a significant benefit to the treatment of persistent wounds and is a major advance over typical smart bandages that attempt to monitor wound condition.’

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom