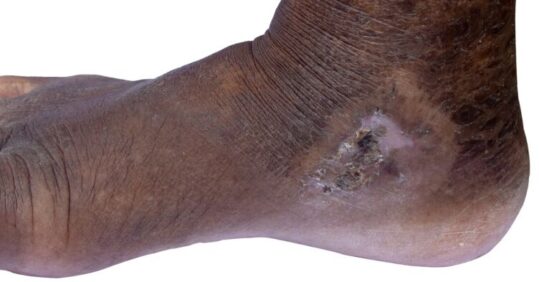
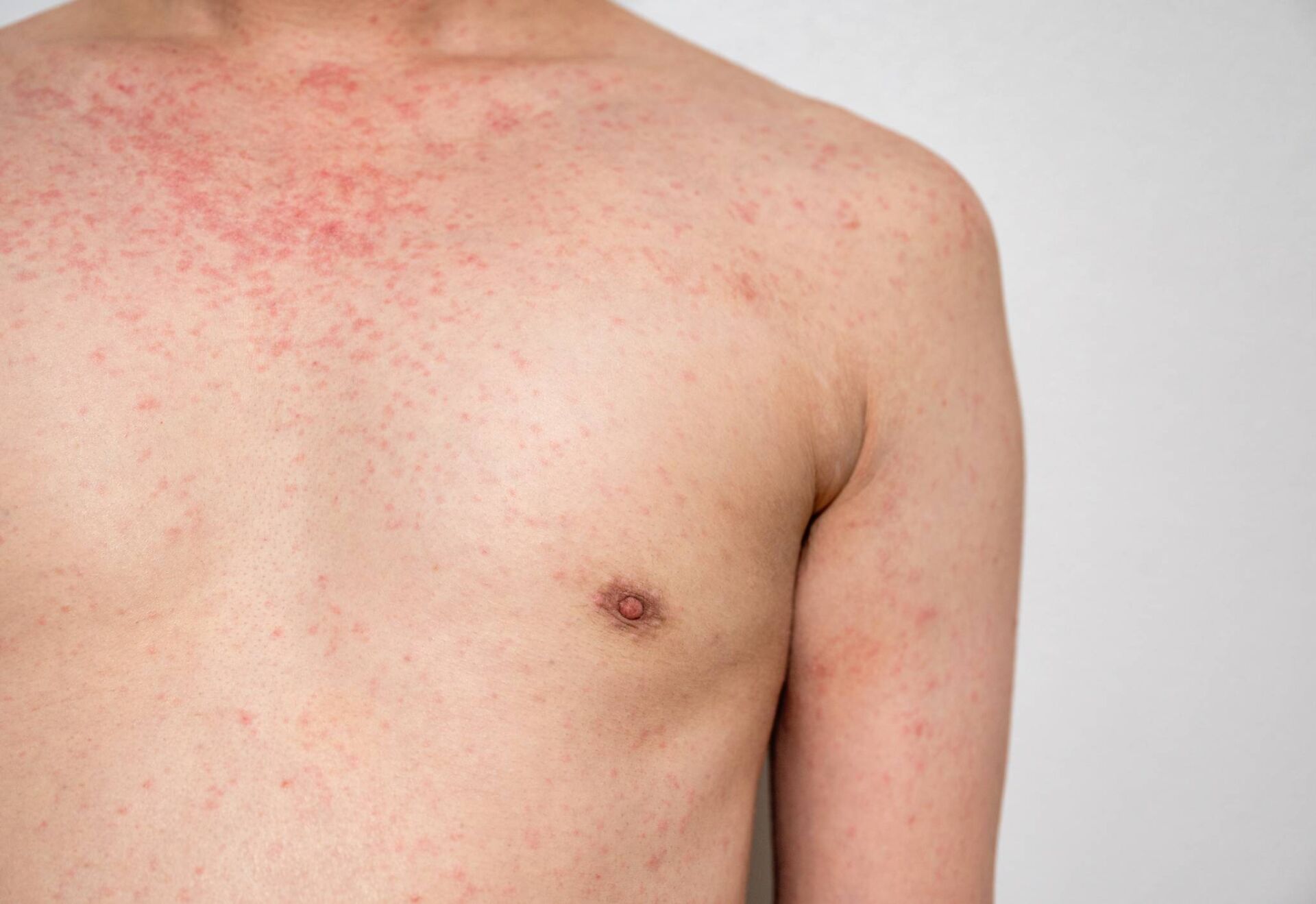
Community nursing and health equity expert Dr Neesha Oozageer Gunowa explains how wounds present differently in people with dark skin tones compared with light skin tones, and offers advice on how to ensure appropriate assessment and management of wounds in people with dark skin tones
This module will improve your understanding of:
- How wounds present differently across the range of skin tones.
- How to assess wounds in people with dark skin tones.
- The place for objective tools and technology to support wound assessment.
- How to implement best practice in wound management for people with dark skin tones.
- Alternative options in wound dressings for people with dark skin tones.
The nursing workforce is required to have the skills to provide safe, equitable and high-quality care at all times and in all settings, based on evidence-based research.
An important area where we still need to address a lack of equitable care is the management of wounds in people with dark skin tones.
For example, we know that patients with dark skin tones are more likely to be diagnosed with pressure ulcers at a late stage, due to early signs of deterioration being missed.
There are expert consensus documents on the assessment and management of wounds in people with dark skin tones. However, further research in this area is still needed to inform best practice.
In the meantime, it is important to recognise our role as nurses in eradicating health inequities in this area, to the best of our abilities.
Assessment of wounds in people with dark skin tones
A comprehensive and accurate wound assessment is crucial to define the status of the wound and helps identify impediments to the healing process.
Wound assessments should involve a thorough inspection of the skin, and this includes documenting a person’s skin tone. Early identification of skin changes is vital to pick up on important signs and prevent skin and tissue breakdown and damage.
However, visual skin changes may be subtle or non-existent in people with dark skin tones. They may vary in colour, for example presenting as purple, grey or blue.
As a result, over the past few years there has been a shift away from the campaign ‘React to Red’. This was an initiative to promote early identification of pressure ulcers, based on a simple reminder that the first sign is redness of the skin. However, the campaign excluded a large proportion of the population with dark skin tones.
Key aspects that should be included in a wound assessment are outlined in Box 1 below.
| Box 1. Key components of a skin assessment – what to consider – How the wound/periwound compares to the surrounding skin – Any variation in colour in the wound/periwound compared with surrounding skin – Variation in temperature across the wound, periwound and surrounding area – Feel of the skin – for example, if firm or spongy to the touch – Surface of the skin – for example, if looks or feels tight or shiny – Any changes in the texture of the skin – Presence of any swelling – Pain, itchiness or changes in sensation |
Author
Dr Neesha Oozageer Gunowa is a Senior Lecturer and Community Pathway Lead at the University of Surrey
Find this learning module
The full module can be found on the Nursing in Practice 365 website
Not a Nursing in Practice 365 subscriber? Register for free or gain access to more CPD modules as a Premium member.