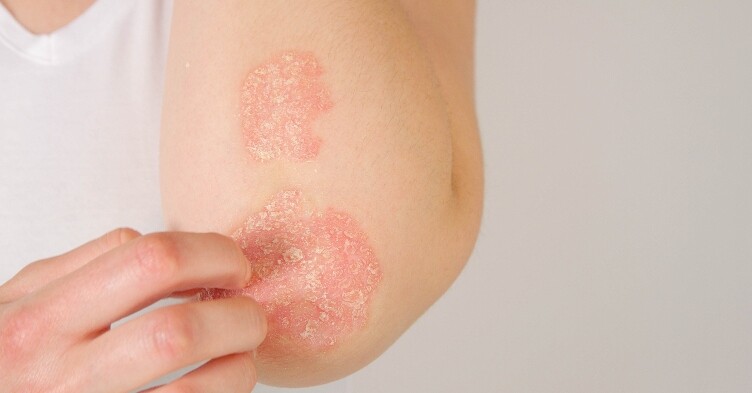
Dealing with skin tears
Key learning points:
- Skin tears are unique acute wounds, affecting the extremes of age and the critically or chronically ill
- Skin tears are preventable but often develop into chronic wounds. The hands, arms and legs are the most common location
- Skin tears should be treated in a systematic way to include: cleansing with normal saline, controlling of bleeding, removing clots and debris, approximating wound edges, and choosing an appropriate dressing for wound bed characteristics
Skin tears are acute wounds generally found in the extremes of age and are often associated with individuals who are critically or chronically ill.1,2
The International Skin Tear Advisory Panel (ISTAP) defines a skin tear as: “a wound caused by shear, friction, and/or blunt force resulting in separation of skin layers. A skin tear can be partial thickness (separation of the epidermis from the dermis) or full thickness (separation of both the epidermis and dermis from underlying structures).”3
Skin tears are traditionally categorised as acute wounds due to the mechanism of injury, which means they should heal in a timely trajectory. However, skin tears frequently fail to meet the expected healing milestones and may develop into a chronic, non-healing wound. This can place a considerable financial burden on healthcare resources. There are also significant effects for individuals who experience a skin tear, in particular pain.4
Prevalence of skin tears
Skin tears are generally more common among individuals in long-term care, with reported prevalence rates ranging from 10-54% across different countries.5-9 Individuals with skin tears are also often seen in the emergency department, with estimates ranging between 0.6%-6.1% per 1,000 attendances.10-13 Prevalence in acute care has been reported between 3.3 and 22%.14-16 The prevalence of individuals with skin tears presenting to their GP practice is unknown but anecdotal evidence suggests that the management of skin tears is commonplace for nurses in primary care.
Related Article: Call for regulatory guidelines as NHS adopts AI in dermatology care
Risk factors for skin tears
The ISTAP conducted a scoping review of risk factors for skin tears and subsequently developed a risk assessment pathway.4 This has three categories:
1. General health (chronic and critical disease, polypharmacy, nutrition, and impairment of sensory, visual, auditory cognition).
2. Mobility (history of falls, impaired mobility, dependent activities of daily living and mechanical trauma).
3. Skin (extremes of age, fragile skin and previous skin tears).
The pathway helps to identify modifiable and non-modifiable risk factors. For this article, two of the risk factors will be examined as they are more commonly seen in primary care.
Age-related skin changes
Physiological skin changes associated with aging are frequently seen over the age of 65 years. These result in a loss of the skin’s mechanical functions.17 Photo aging (elastosis) is an extrinsic cause that potentiates age-related skin changes.18,19 Current evidence supports that fragile aging skin is a chronic condition and that factors for increased risk of skin tears include:
- Being a Caucasian over the age of 65 years.
- Presenting with skin exhibiting signs/symptoms of aging or sun damage.
- Having any of the deficits in the categories in the ISTAP risk assessment pathway.4-9
More recently, Lewin et al20 reported six key factors that were linked to an increased risk of skin tear development:
- Ecchymosis.
- Senile purpura.
- Haematoma.
- Evidence of previous healed skin tears.
- Oedema.
- Inability to independently reposition.
The terms ecchymosis and senile purpura are frequently used interchangeably by healthcare professionals.21 Ecchymosis can be defined as bruised skin in the absence of dry, sun-damaged (photoaged) or pigmented (haemosiderin-stained) skin.21 Ecchymosis is the result of bleeding into the subcutaneous tissue which is not related to a traumatic event but rather a pathophysiologic cell function.22-24
Senile purpura, in contrast, is a common condition frequently seen on forearms and legs of older individuals. The cause has been linked to the loss of subcutaneous tissue and capillary fragility, and it is hypothesised to be linked to the excessive use of aspirin or other blood thinners; however, this has not been tested empirically.22,23 Senile purpura appears as a bruise-like appearance on aging, dry, sun-damaged or pigmented (haemosiderin-stained) skin.21
Stellate spontaneous pseudoscars present as thin white scars found in the aging skin and are normally found on the back of hands and the radial and extensor aspects of the forearms.22 The clinical appearance is that of multiple, whitish, slightly depressed, irregularly shaped frequently linear or star-shaped areas in an atrophic and irregularly pigmented skin. Senile purpura is commonly found in combination with pseudoscars.17,22,23
Areas of frequent sun exposure (posterior forearms, pretibial area, dorsal hands, pre-sternal area and scalp) are reported to be the areas that demonstrate dermatoporosis.17,22
Polypharmacy
The use of multiple medications that might cause interactions, reactions or confusion is common among older adults.24
Polypharmacy has also been indicated as an independent risk factor for falls.25 Pervin24 concluded that individuals receiving four or more medications are at a greater fall risk. Both these factors24 link polypharmacy to a potential heightened risk of skin tears.3 Medications that may affect the skin include:3
Related Article: Abdominal body fat is a higher risk for developing psoriasis
- Antibacterial agents.
- Antihypertensives
- Analgesics.
- Tricyclic antidepressants.
- Antihistamines.
- Antineoplastic agents.
- Neuroleptics.
- Diuretics.
- Hypoglycemic agents.
- Nonsteroidal anti-inflammatory agents.
- Oral contraceptives.
- Steroids.
Anatomical location of skin tears
Existing evidence suggests that skin tears occur primarily on the extremities.3,26,27
The early study by Payne and Martin reported that 22% of skin tears occur on the lower extremities, 65% on the arms and 13% on hands.26
A Canadian study in a long-term care facility reported 46% of skin tears occur on the lower extremities, 43% on the arms and 11% on hands.9 A more recent study in Japan reported that the majority (83%) of skin tears occurred on the hands and arms.27 Further studies are required to establish if skin tears occur in other anatomical locations to ensure that all risk factors are explored and prevention strategies established.
Skin tear classification
Classification with common and appropriate descriptors enables healthcare professionals to more effectively communicate with other healthcare professionals, policy makers, researchers and patients.28 The ISTAP system is the only published system to demonstrate reliability, validity and utility for skin tear classification in clinical practice and research,29,30 although it has yet to be validated in primary care. The ISTAP system involves three skin tear types:
Type 1 – no skin loss.
Type 2 – partial skin loss.
Type 3 – complete skin loss.29
The ISTAP system underwent test-re-test reliability with the expert ISTAP panel and inter-rater reliability testing with 339 healthcare professionals. They reported a level of agreement sufficient to indicate they had met their objective of developing a reliable and valid skin tear classification system.29 A second study has validated the use of the ISTAP classification system with 270 healthcare professionals.30
Dressing selection
ISTAP has established a global product selection guide (Table 1) to identify products that allow for moist wound healing in accordance with the wound conditions, and respecting the fragile nature of the skin.31 The list is neither all-inclusive nor all encompassing. Frequency of dressing changes will be based on local conditions and facility policy. ISTAP recognised that not all of the products discussed are available in all countries. The list is the result of a systematic review by an international group of healthcare professionals.
Hydrocolloid and film dressings were excluded because of their strong adhesive nature. Iodine-based dressings were excluded for their drying effects.
Medical honey dressings were excluded because of the increased risk of peri-wound maceration.31 In a recent publication32 reported that Leptospermum honey-based dressings were effective in managing skin tears while respecting fragile peri-wound skin. They are available in various formats, including alginates and hydrogels.33 Both alginates and hydrogels were included in the ISTAP product selection guide, so healthcare professionals may want to consider Leptospermum honey dressings if appropriate for the wound bed environment.
Polyhexamethylene biguanide (PHMB) dressings were excluded because of a lack of availability of non-gauze forms in many countries.31 PHMB is an effective antimicrobial agent and is incorporated in a range of wound products including gels, non-adherent contact layers, foams and gauze dressings.34 Hydrogels, non-adherent contact layers and foams were included on the ISTAP product guide and as PHMB is claimed to be an effective antimicrobial product, healthcare professionals may want to consider its use if appropriate for the wound bed conditions. There have been no studies to date addressing the use of PHMB for the treatment of infected skin tears.
Wounds closed by primary intention are traditionally secured with sutures or staples, however given the fragility of elderly skin, sutures and staples are not recommended.3,23 Expert opinion also suggests that use of adhesive strips (Steri-Strips) may increase the risk of further skin injury, and while more research is needed, case studies and expert opinion suggest that adhesive strips are no longer a preferred treatment option for skin tears.23,31,35,36
Skin tears should be managed in a systematic way to include: cleansing with normal saline, controlling of bleeding, removing clots and debris, approximating wound edges, and choosing an appropriate dressing to address wound bed characteristics.
Best practice supports that a skin flap (the pedicle) should be approximated to the extent possible, and topical dressings should be chosen and applied.31,36 Always remove the dressing with the pedicle, not against it, to maintain flap viability. Indicate on the dressing the classification, size and shape of the skin tear and direction for dressing removal. If the skin tear is infected or extensive, a wound care specialist should assess.23,31,35-36
Related Article: CPD: Case by case – acute and emergency dermatology presentations
Conclusion
Skin tears are unique and preventable acute wounds affecting the extremes of age and the critically or chronically ill. They are highly likely to develop into chronic wounds and impose health burdens on individuals and healthcare services. Although often under-reported and minimised by the healthcare community, skin tears are thought to be highly prevalent and troublesome for the elderly population and are reported to negatively impact an individual’s quality of life.
References
1. Bank DN, Nix D. Preventing skin tears in a nursing and rehabilitation center. Ostomy Wound Management 2006;52(9):38-46.
2. Baranoski S, Ayello E, Tomic-Canic M, Levine J. Skin: An essential organ. Wound care essentials: Practice principles 3rd ed, 2012.
3. LeBlanc K, Baranoski S, Christensen D, Langemo D, et al. Consensus statements for the prevention, prediction, assessment and treatment of skin tears. Advances in Skin and Wound Care 2011;24(9):2-15.
4. LeBlanc K, Baranoski S, Christensen D, Langemo D, et al. A tool kit to aid in the prevention, assessment, and treatment of skin tears using a simplified classification system. Advances in Skin and Wound Care 2013;26(10):459-476.
5. Everett JS, Powell T. The underestimated wound. The Australian Journal of Wound Management 1998;2(8):8-30.
6. McErlean BS. Skin tear prevalence and management at one hospital. The Australian Journal of Wound Management 2004;12(2):83-88.
7. Santamaria N. Identifying the prevalence of wounds within western Australia’s public health system. EWMA Journal 2009;9(3):13-18.
8. Woo K, LeBlanc K. Prevalence of skin tears among the elderly living in Canadain long-term care facilities. Canadian Assoication of Wound Care, 2014.
9. LeBlanc K, Christensen D, Cook J, Gutierrez O. Prevalence of skin tears in a long-term care facility. Journal of Wound, Ostomy & Continence Nursing 2013;40(6):580-584.
10. Ball C. The management of pretibial lacerations in the community. Journal of Community Nursing 2002;16(6):37-42.
11. Davis A, Chester D, Allison K, Davidson P. A survey of how region’s A&E units manage pretibial lacerations. Journal of Wound Care 2013;13(1):5-7.
12. McClelland HM, Stephenson J, Ousey K, Gillibrand WP, Underwood P. Wound healing in pre-tibial injuries – an observation study. International Wound Journal 2012;9(3):303-310.
13. Kennedy P, Kerse N. Pretibial Skin Tears in older adults: A 2-year epidemiological study. Journal of the American Geriatrics Society 2011;59(8):1547-48.
14. Chang Y, Carville K, Tay A. The prevalence of skin tears in the acute care setting in Singapore. International Wound Journal, 2016.
15. Strazzieri-Pulido KC, Peres G, Campanili T, Conceição de Gouveia Santos V. Skin tear prevalence and associated factors: a systematic review. Rev Esc Enferm USP 2015;49(4):668-674.
16. Strazzieri-Pulido KC, Conceição de Gouveia Santos V, Carville K. Cultural adaptation, content validity and inter-rater reliability of the STAR Skin Tear Classification System. Emfermagem 2015;23(1):155-61.
17. Kaya G, Saurat J. Dermatoporosis: A new concept in skin aging. European Geriatric Medicine 2010;1(4):216-219
18. Fore J. A review of skin and the effects of aging on skin strucutre and function. Ostomy Wound Management 2006;52(9):24-35.
19. Koyano K, Nakagami G, Iizaka, S, Minematsu T, et al. Exploring the prevalence of skin tears and skin properties related to skin tears in elderly patients at a long-term medical facility in Japan. International Wound Journal 2016;13(2):189-97.
20. Lewin G, Newall N, Alan J, Carville K, et al. Identification of risk factors associated with the developemnt of skin tears in hospitalized older persons: a case-control study. International Wound Journal, 2015.
21. Newall N, Lewin G, Bulsara M, Carville K, et al. The development and testing of a skin tear risk assessment tool. International Wound Journal, 2015.
22. Kaya G, Saurat J. Dermatoporosis: A chronic cutaneous insufficiency/ fragility syndrome. Dermatology 2007;215(1):284-94.
23. Rayner R, Carville K, Leslie G, Roberts P. A review of patient and skin characteristics associated with skin tears. Journal of Wound Care 2015;24(9):406-14.
24. Pervin L. Polypharmacy and the aging: Is there cause for concern? AJN 2008;1(1):10.
25. Hajjar E, Cafiero A, Hanlon J. Polypharmacy in elderly patients. American Journal of Geriatric Pharmacotherapy 2007;5(4):345-51.
26. Payne RM. Skin tears, the epidemiology and managment of skin tears in older adults. Ostomy Wound Management 1990;26(1):26-37.
27. Sanada H, Nakagami G, Koyano Y, Iizaka S, Sugama J. Incidence of skin tears in the extremities among elderly patients at a long-term medical faciltiy in Japan. Geriatric Gerontology International 2015;15:1059-61.
28. Salcido R. The language of wound care: taxonomy of discourse. Advances in Skin and Wound Care 2000;13(1):252-245.
29. LeBlanc KB, Baranoski S, Holloway S, Langemo D. Validation of a new classification system for skin tears. Advances in Skin and Wound Care 2013;26(6):263-265.
30. Skiveren JB, Bermark S, LeBlanc K, Baranoski S. Danish Translation and validation of the international skin tear advisory panel skin tear classification system. Journal of Wound Care 2015;24(8):388-92.
31. LeBlanc K, Baranoski S, Christensen D, Langemo D, et al. The art of dressing selection: A consensus statement on Skin Tears and Best Practices. Advances in Skin an Wound Care 2016;29(1):32-46.
32. Johnston C, Katzman M. A Clinical Minute: Managing Skin Tears with Medihoney. Ostomy Wound Management 2015;61(6).
33. Acton C, Dunwoody G. The use of medical grade honey in clinical practice. British Journal of Nursing 2008;17(20):S38-S44.
34. Butcher M. PHMB: an effective antimicrobial in wound bioburden management. British Journal of Nursing 2012;21(12) S16-21.
35. Holmes R, Davidson M, Thompson B, Kelechi T. Skin Tears: Care and management of the older adult at home. Home Healthcare Nurse 2013;31(2):90-103.
36. Ellis R, Gittins E. All Wales Rissue Viability Nurse Forum Best Practice Statement The Assessment and Management of Skin Tears. Wounds UK, 2015.

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom