Lack of nurses ‘most concerning’ shortage in NHS, report finds
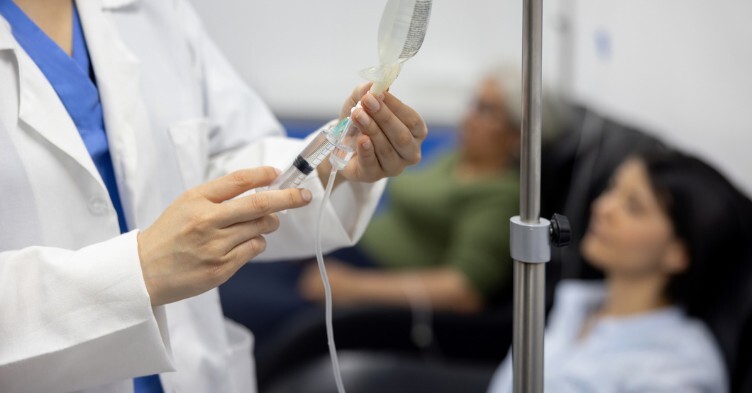
The nursing staff shortfall is the ‘most concerning’ shortage across the NHS, a report published this week by NHS Providers – a membership organisation for NHS trusts – has found.
The report, ‘The state of the NHS Provider sector’, pointed out that the Health Foundation, The King’s Fund and the Nuffield Trust have projected that on current trends, in 10 years’ time, the NHS will have a shortfall of 108,000 full-time equivalent nurses. Additionally, successful applications to undergraduate nursing courses have lagged behind government targets, with the number of placed applicants in 2018 4% lower than in 2016.
It also raised concerns around the exodus of nurses from the European Union (EU) with 1,584 more nurses and health visitors from EU countries leaving their roles than joining them between July 2017 and July 2018.
Related Article: Increase in ARRS nursing roles despite total staff drop
The migration advisory committee recommended that nurses should remain on the shortage occupation list in May 2019 but later decided to review salary thresholds and a potential points-based future immigration system.
The report warned: ‘The criteria for “points” in a future system, and the overall nature of migration into the UK from 2021 and beyond, is unclear.’
A shortage of nurses, it said, may significantly affect the quality of patient care, with increased waiting times, potential risks to patient safety and patient experience.
However, the report went onto feature ‘innovative’ recruitment and retention approaches. This includes a health and care workforce strategy to help address workforce challenges across ten localities within Greater Manchester.
Meanwhile, six trusts in the west Yorkshire and Harrogate integrated care system collaborated to introduce staff passports in order to more easily share staff, and trusts in south Yorkshire and Bassetlaw use a shared nursing bank.
Related Article: NMC to pitch code and revalidation changes to governing council
Yeovil District Hospital NHS Foundation Trust has been recruiting nurses from Dubai and the Philippines successfully for the past two years, without outsourcing, and is now supporting 12 other trusts with international recruitment.
Responding the report, RCN chief executive and general secretary Dame Donna Kinnair said: ‘Ministers should be honest with the public about the scale of the challenge but they should also prepare to answer the difficult questions that will follow on how they are going to turn it around, and almost six in 10 (59%) were worried this was not in place.
‘Public awareness of these issues, especially staff shortages, is already high but so are their levels of anxiety. Rose-tinted spectacles, nostalgia or political spin will not cut it when patients and taxpayers are concerned about how safe things currently are at their local hospital or service.
Related Article: New ‘life-extending’ drug for ovarian cancer added to NHS
‘This report is absolutely right to call for a funded and credible workforce plan for England that addresses the shortage of at least 40,000 nurse jobs. It clearly states that nursing workforce shortages are the most concerning staffing pressure in the entire health service. This should be seen in the context of a massive shortage across all health and care settings, and all sectors of provision.
‘Now that the NHS in England has officially asked Government to address the question of accountability for workforce supply and planning, it is clear that legal duties must be introduced into legislation. This is in addition to an investment of at least £1 billion per year extra in nursing higher education.’

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom


Nursing staff shortages are the ‘most concerning’ across the NHS, a report published this week by NHS Providers – a membership organisation for NHS trusts – has found.