Long Covid ‘one of the most serious’ impacts of pandemic on nurses
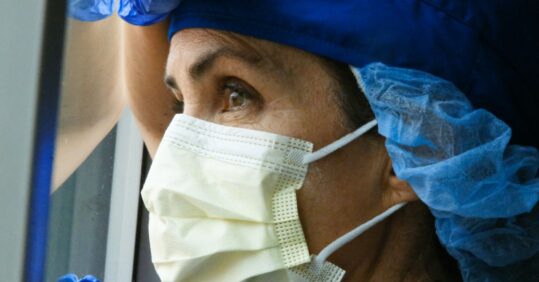
Long Covid has been described as one of the ‘most serious’ negative impacts of the pandemic on nurses, during a latest round of submissions to the Covid-19 public inquiry.
The Royal College of Nursing (RCN), represented by Fennella Morris KC in this week’s preliminary inquiry meeting, highlighted how a ‘significant body of nurses have been left with chronic ill health’ following their ‘committed service to the community at a time of national crisis’.
As part of its submission to Module 3 of the UK Covid Inquiry, which will look into the governmental and societal response to Covid-19, and dissect the impact the pandemic had on healthcare systems, the RCN described how nurses with long Covid have been left ‘unable to work and their lives are permanently blighted’.
During a preliminary inquiry hearing on Wednesday, Ms Morris KC affirmed that the RCN ‘adopts and supports’ the Trades Union Congress’s proposal that long Covid be designated a disability in law, in order that those who suffer with long Covid may be ‘properly protected.’
Related Article: New preceptorship package for social care nurses
Going further, she said the RCN was asking that a compensation scheme be ‘set up soon,’ without waiting for the end of the inquiry, ‘to meet the needs of those healthcare workers who are chronically ill as a result of long Covid, and who cannot work as they did before’.
RCN members ‘went to work with a daily fear of dying’, Ms Morris KC commented, adding that many ‘did not get to see their own children for months apart from some distance’, as they ‘lived in fear’ they could bring the infection home.
Short staffing meant nurses were looking after ‘significant’ numbers of patients which ‘far exceeded’ the nurse-to-patient ratio, she said, emphasising that ‘this was a patient safety risk’, with nurses ‘concerned a patient could deteriorate or die in one of the rooms without them knowing’.
Thousands of nurses worked with ‘inadequate [personal protective equipment], on understaffed wards, with inadequate training, risk assessments or support, while their own physical and mental health suffered,’ Ms Morris KC said, ‘causing them to hit breaking point’ and ‘doubt whether they were able to continue a career in nursing’.
She added that ‘the long-term failure by successive governments to invest in the nursing workforce meant health and care services were chronically under-resourced to deal with the pressures of the pandemic’.
RCN members ‘repeatedly’ told the professional body that staffing levels were ‘challenging and, in many instances, unsafe’, Ms Morris KC said, but that this was ‘a state of affairs’ that preceded the pandemic.
Related Article: Applications to study nursing in England at ‘new low’
It is a ‘key theme’ of the submissions of the RCN is that recommendations from the inquiry should include ‘a strong legislative underpinning of government accountability for workforce planning and supply across the health and social care service, and a commitment to development of a sustainable nursing workforce if our country is to respond to a future pandemic’, Ms Morris KC added.
The development of a sustainable workforce supply can be achieved through ‘a fully-funded workforce strategy for recruitment and retention and ongoing assessment of workforce requirements in health and social care’, the RCN has suggested.
Ms Morris KC warned that ‘the failure of the UK Government to tackle the issues facing the nursing workforce, including in recruitment, retention and burnout, remains a serious risk to the country’s ability to robustly tackle future pandemics’.
The Module 3 hearings of the Covid Inquiry are scheduled for 10 weeks in autumn 2024.
Related Article: Paul Rees appointed as permanent NMC chief executive and registrar
Ms Morris KC highlighted that RCN chief executive and general secretary Pat Cullen will give evidence to the inquiry around the ‘heavy burden’ of the Covid-19 pandemic on nursing staff working in hospitals, care homes, general practice, the community and beyond.

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom




