The NHS is failing to assess people with rheumatoid and early inflammatory arthritis quickly enough, a clinical audit has shown.
A report of the NHS’s performance against seven standards of high-quality care for people with early or inflammatory arthritis (EIA) found that many patients in England and Wales are experiencing long waiting times and delays following a GP referral.
Quality standards set by the National Institute for Health and Care Excellence (NICE) state that patients should receive a referral from a GP within three days and assessment in a rheumatology service within 3 weeks of that referral.
However, according to the report only 20% of people who see a GP with suspected rheumatoid or EIA are referred to rheumatology specialist services within three days.
Furthermore, only 37% of people referred with suspected rheumatoid arthritis or EIA are seen by a specialist within three weeks.
The National Rheumatoid and Early Inflammatory Arthritis Audit report also found considerable variation in healthcare provision for people with EIA across the country.
For example, people in Wales are half as likely to see a specialist within three weeks as those living in London.
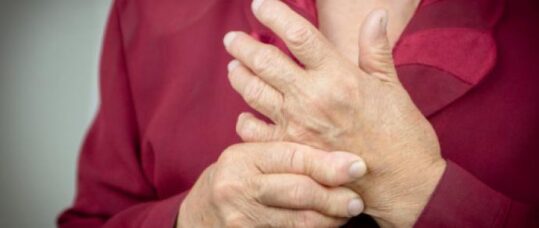
Rheumatoid arthritis and EIA are conditions in which the immune system attacks the joints, making them inflamed and can lead to long-term joint damage causing pain and disability.
Therefore, early referral, assessment by rheumatology services and targeted treatment are vital to rapidly control disease and minimise long-term joint damage, which EIA can cause.
To help facilitate better referral times, the report is recommending greater training and support for healthcare professionals in primary care to raise awareness of early symptoms and signs of inflammatory arthritis and the importance of early referral and diagnosis.
Dr Liam O’Toole, chief executive officer of Arthritis Research UK, said: “The results of this audit are disappointing and show that people with inflammatory arthritis still aren’t getting the treatment they need fast enough.
“The impact of delayed treatment can be detrimental and life-changing; four out of five people with inflammatory arthritis are at risk of long-term disability or reduced life expectancy because of delays.
“We urge that immediate action is taken to improve access to these services, so that people with inflammatory arthritis get the treatment they need and the quality of life they deserve.”
Ninety-seven per cent of NHS rheumatology providers in England and Wales were registered to participate in the audit, which collected data from 5,002 patients in England and Wales.
The audit was performed by British Society of Rheumatology, Northgate Public Services and the MRC Lifecourse Epidemiology Unit at the University of Southampton between 1 February 2015 and 30 October 2015.