How nurses can help support uptake of cancer screening post-Covid-19
Cancer Research UK GP Dr Stephanie Edgar and Cancer Research UK early diagnosis manager Rachael Ogley explain what community and practice nurses need to know about the national cancer screening programmes, and what can be done in primary care to support people to access these services.
Cancer screening involves testing apparently healthy, asymptomatic people for signs of the disease. It can detect cancers at an earlier stage and in some cases prevent them from developing in the first place, by picking up cellular changes that, if left, could progress into the disease.
In the UK there are three screening programmes covering breast, cervical and bowel cancer.
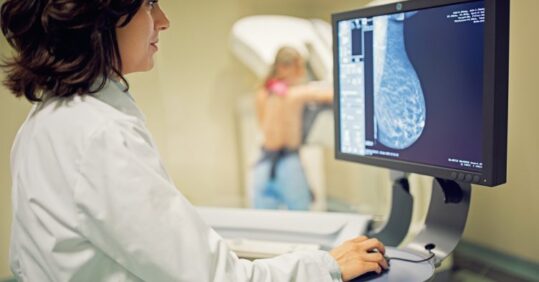
Breast screening is offered to women aged 50–70 and involves a mammogram on a three-yearly cycle.
Cervical screening is offered to women from the age of 25–64 years. The frequency of this varies across the UK and can vary from 3–5 years depending upon the women’s age and where she lives – check local guidance to find out what applies within your area of work.
Cervical screening involves a smear test to check for abnormalities in the cells of the cervix and to test for a virus called human papilloma virus (HPV). High risk strains of HPV can cause cervical cells to become abnormal. Most cases of cervical cancer are linked to high risk-HPV. Cervical screening also applies to anyone within this age range who have a cervix, including trans men and non binary people.
Bowel screening is offered every two years to all men and women who are registered with a GP and aged 60-74 in England, Wales and Northern Ireland and age 50-74 in Scotland. Scotland, England and Wales use the faecal immunochemical test (FIT) as the screening test. Northern Ireland currently use the guaiac faecal occult blood test but have plans to move over to FIT. The test kit is sent to people to complete in the privacy of their home. FIT is a more sensitive test, and also has the advantage of needing only one stool sample. This may be one of the reasons why uptake is higher with FIT. The test involves the detection of microscopic blood within a stool sample, and if the result is positive leads to further investigations.
Each of the cancer screening programmes have been shown to reduce deaths from the cancer in question and give the best chance of being diagnosed with early stage disease, but as with all screening, there are harms as well as benefits of taking part. Harms include the risk of overdiagnosis – where a cancer is diagnosed that would not have gone on to cause harm in the person’s lifetime – anxiety, and false negative results. Information about this is provided with the literature that people receive when invited for screening.
Related Article: Research raises questions about vitamin D and calcium supplements for fracture prevention
For more information about each cancer screening programme and the associated benefits and risks see the Cancer Research UK website.
How has Covid-19 affected cancer screening?
Since the start of the lockdown, around 3 million fewer people have been screened via the bowel, breast or cervical cancer screening programmes in the UK than we would expect under normal circumstances.
Cancer screening services have started to resume across the UK, with some variation across nations.
As invitations are sent and follow up tests resume, there will be perceived risks as well as emotional and physical barriers to attending appointments for patients. Practice staff are in an ideal position to reassure patients of the safety measures in place for cervical screening as well as informing patients about participating in bowel and breast screening.
Screening programmes are for people who are asymptomatic. It is important to remember that if patients have symptoms, they must see their GP to discuss these further to allow assessment, investigation and referrals if needed, even if they have had a recent negative screening test.
What can you do to support your practice population?
Practices should consider focusing on particular groups of people who tend to be less likely to take part in cancer screening generally. Evidence suggests that uptake is lower in those from ethnic minority communities and vulnerable groups, such as those with learning disabilities, although gaps in data availability persist. See Cancer Research UK’s health professional web content for information about how practices might get involved in identifying and supporting people to participate.
Cervical screening
Over the past 10 years there has been a decline in the number of women taking up their offer of cervical screening. The reasons for non-attendance are complex and several factors may be at play, including lack of knowledge, communication difficulties, lack of perceived time or the inflexibility of practice appointment times. Understanding who is not attending screening and the barriers preventing them from participating is important when looking at ways to support engagement with the programme.
There are a range of different things that practice nurses and the wider team can do to help support informed uptake, from raising screening opportunistically with women who are in for other clinics, like travel vaccinations, blood tests or asthma checks, to more comprehensive approaches to identify and proactively reach out to people who’ve not taken part. For more information on this see CRUK’s page on increasing cervical screening uptake.
For some women, barriers to participation may be exacerbated by Covid-19 and practices may need to consider how they can proactively raise awareness of screening invitations and new practice processes to encourage informed participation. This might include assuring patients what safety measures are in place to keep them safe and how their experience might differ to what they’re used to.
Some suggested measures include:
- Primary care providers should start to review their local records or use final non-responder lists to identify individuals whose screening may have been affected by Covid-19 (for example, their appointment has been cancelled and not been rebooked, they have been refused an appointment during the pandemic response, they have not responded to a reminder letter) and be proactive in contacting them about their screening and giving them the opportunity to attend.
- Consider the length of appointment time to allow for the cleaning of the room after each patient and the use of PPE. Assure patients what safety measures are in place to keep them safe.
- Consider running a separate screening clinic as opposed to alongside normal treatments.
- Increasing accessibility, for example, by arranging screening clinics at the weekend or in evenings, may address barriers to participation for some.
- Inform patients about what to expect if they do attend. Those that prefer not to attend at the moment should be safety netted, including being given information about what health changes aren’t normal, so they recognise when they need to access care.
Further information on how you can support people is available from the Cancer Research UK cervical screening page.
Related Article: District nurse referral forms reviewed after coroner’s concerns over patient death
Breast and bowel screening
It is important that nurses have good knowledge about each screening programme to enable them to have opportunistic conversations with patients. All practice staff should to be able to explain what happens for each one – including the benefits and harms of taking part – as well as encouraging patients to read the information that comes with their invitation to help them make an informed choice about participation.
Last year the test used for Bowel Cancer Screening changed. See Cancer Research UK’s Bowel Screening Good Practice Guide and other helpful resources on the bowel screening hub such as a video on how to do the test and more information about the FIT screening test.
It is also important to understand the key differences in the use of FIT for screening asymptomatic people through the bowel screening programme, in contrast to its use to investigate symptomatic patients. Have a look at our FIT key differences infographics.
Practices should at the present time be particularly alert to those individuals who may have received a positive breast or bowel screening result and are awaiting a follow-on test, or who have had their initial bowel and breast screening invitations delayed due to Covid-19.
Primary care schemes to improve screening uptake
In England and Northern Ireland, cervical screening uptake is incentivised through the Quality and Outcomes Framework (QOF) – practices need to ensure a high proportion of the target cohort undergo screening regularly to receive payment.
Additionally, in England the QOF Quality Improvement module on the early diagnosis of cancer, introduced this year, provides an opportunity for GP practices to develop quality improvement plans for all screening programmes. This was to involve reviewing the practice’s screening uptake and potential inequalities, and work with local public health and cancer teams to come up with an improvement plan, and Cancer Research UK has developed resources to support practices in this. However, given the impact Covid-19 has had on screening programmes, and NHS England has now revised this module to focus in particular on restoring uptake of cervical screening and ensure patients are aware they can access primary care safely.
There are currently no other national incentive schemes operating in other parts of the UK, but this may change in the future. Even without such incentive schemes in place, it’s important to remember the valuable role that primary care can play in helping to support informed uptake of screening, removing barriers, reaching out to communities that national organisations can find it difficult to reach.
Related Article: New learning disability nursing network launched by QICN
What additional support is available?
You can contact our Early Diagnosis Team for further information.
Cancer Research UK offers free, individualised support for your practice or Primary Care Network, and your local Cancer Research UK Facilitator will be able to support you in identifying interventions to help improve your screening uptake which will be tailored to your specific needs.
Cancer screening offers the best chance of being diagnosed with earlier stage cancer and saves thousands of lives each year. The pandemic has brought some challenges, but it’s vital that cancer screening gets back on track as quickly and as safely as possible. And for the future, researchers are looking for new tests and new ways to spot cancers early, in the hope that more people, across a wider range of cancer types, can benefit.

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom




