All type 1 diabetes patients to be offered continuous glucose monitors in England
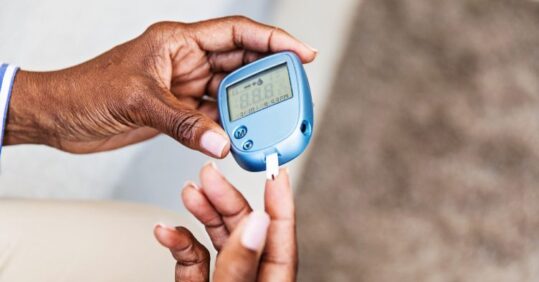
All type 1 diabetes patients will become eligible for real-time or ‘flash’ glucose monitors, with the devices to be prescribed by their general practice or local diabetes team, NHS England has announced.
NICE today confirmed clinical guidance, previously published in draft form, recommending this type of continuous diabetes monitoring should become the norm for all adults with type 1 diabetes, and some with type 2.
NHS England confirmed this will be rolled out across the country, as a result of the announcement.
The recommendations, which also apply to children and young people with type 1 diabetes, will mean ‘more than 250,000’ people are offered the new technology and decrease the need for finger-prick testing by ‘up to’ 50%, said NICE.
Previously, NICE had only recommended continuous glucose monitoring technology for adults with type 1 diabetes in certain circumstances.
The two types of technology that will be available to patients are:
Related Article: Research insights: the latest updates from clinical papers
- Real-time continuous glucose monitoring (rtCGM), where a sensor attached discreetly to the person’s body collects data on current and previous glucose levels and transmits it to their smartphone, as well as a prediction of where the levels are headed. These provide optional alarms or alerts warning users of immediate and/or impending high or low blood sugar.
- Intermittently scanned continuous glucose monitoring (isCGM, commonly referred to as ‘flash’)’, where users scan a sensor on their arm to obtain blood sugar data. Not all of these provide optional alarms or alerts.
NHS England has already rolled out NICE-recommended flash devices to around 50% of those with type 1 diabetes, against an original target of 20% by this month in the NHS Long-Term Plan, said NICE.
NICE centre for guidelines director Dr Paul Chrisp said the recommendations ‘will be a step forward in helping all people with type 1 diabetes manage their condition’.
‘Many people find finger-prick testing to be painful and time-consuming and the introduction of technology for all people living with type 1 diabetes will reduce this considerably,’ he added.
Diabetes UK chief executive Chris Askew said the ‘landmark’ guidelines would be ‘transformational for people living with diabetes’.
Meanwhile, National NHS specialty adviser for diabetes Professor Partha Kar said the announcement was ‘the biggest step forward for type 1 diabetes care in years’, allowing ‘everyone eligible to have one of these easy to use pieces of tech if they want to’.
He added: ‘I am delighted to see NICE endorse the use of this technology. These monitors are a win-win – they support diabetes patients to live healthier lives, reduce their risk of hospitalisation while also helping to reduce pressure on NHS services and provide better value for money for taxpayers.’
It comes as a Government-funded study this week revealed 18,000 people have avoided developing type 2 diabetes thanks to the NHS prevention programme.
What do the guidelines recommend?
The new NICE guidance on diagnosing and managing adults with type 1 diabetes said clinicians should ‘offer adults with type 1 diabetes a choice of real-time continuous glucose monitoring (rtCGM) or intermittently scanned continuous glucose monitoring (isCGM, commonly referred to as ‘flash’)’.
This should be based on the patient’s ‘individual preferences, needs, characteristics and the functionality of the devices available’, it added.
Related Article: Half of women with gestational diabetes report facing stigma
The guidance set out that clinicians should also ‘consider’ various factors such as device accuracy and ease of use and frequency and severity of hypoglycaemia.
Another updated NICE guideline on type 2 diabetes in adults also recommended extending the use of ‘flash’ monitoring to adults with type 2 diabetes on ‘multiple daily’ insulin therapy in certain conditions.
These are those who:
Have recurrent hypoglycaemia or severe hypoglycaemia;
Have impaired hypoglycaemia awareness;
Have a condition or disability (including a learning disability or cognitive impairment) that means they cannot self-monitor their blood glucose by capillary blood glucose monitoring but could use an isCGM device (or have it scanned for them);
Would otherwise be advised to self-measure ‘at least’ eight times a day.
‘Flash’ monitoring – or isCGM – should also be offered to ‘adults with insulin-treated type 2 diabetes who would otherwise need help from a care worker or healthcare professional to monitor their blood glucose’, NICE said.
And real-time continuous glucose monitoring (rtCGM) should be considered as ‘an alternative to isCGM for adults with insulin-treated type 2 diabetes if it is available for the same or lower cost’, it added.
The guidance said clinicians should ‘monitor and review the person’s use of CGM as part of reviewing their diabetes care plan’.
The recommendations for those with type 2 diabetes would make the technology available to ‘around 193,000 people’, NICE said.
Related Article: Type 2 diabetes treatment updates: putting NICE into practice
The guidelines also recommended:
Offering SGLT2 inhibitors to a wider group of adults with type 2 diabetes, based on a cardiovascular risk assessment
Considering relaxing the target HbA1c level ‘on a case-by-case basis and in discussion with adults with type 2 diabetes’
A version of this article was originally published on Nursing in Practice sister publication Pulse.

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom




