NICE recommends NHS apps to assess patients for weight-loss medication
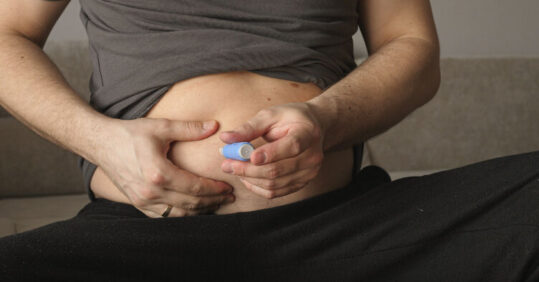
NICE has recommended four digital platforms to be used by NHS weight management services to help assess patients and prescribe weight-loss medication for obesity.
Draft guidance has proposed the use of platforms that can help clinicians support patients psychologically, provide monitoring, and even allow prescription.
The platforms put forward – Liva, Oviva, Roczen, and Second Nature – can be used via an app or on a computer, and NICE has said this will improve accessibility for the many patients living in areas where there are no services or long waiting lists.
Up to 48,000 people would be able to access the virtual care and if all those eligible enrolled, up to 145,000 hours of clinician time would be saved, according to NICE’s calculations.
Prescription of drugs like semaglutide (marketed as Wegovy) and liraglutide is enabled by some of the platforms, while others can collect and share data which helps NHS teams in prescribing decisions.
Related Article: Wegovy weight-loss injections approved by NHS
To be referred patients should meet the criteria for accessing weight management medication, NICE said, meaning they have at least one weight-related comorbidity such as diabetes or high blood pressure, and a body mass index (BMI) of at least 35.0 kg/m2, or at a lower threshold in certain circumstances.
The draft guidance said: ‘Some programmes offer medication reviews with a prescribing clinician alongside regular reviews with other members of the programme’s MDT. Other programmes can collect and share medication adherence data with the NHS team to support weight-management medication prescribing. The frequency of reviews may vary depending on the technology, user preference and stage of the programme.’
NICE has emphasised that medications prescribed through the platforms must be delivered alongside lifestyle changes such as a reduced-calorie diet and increased physical activity.
NICE will collect evidence on the long-term cost effectiveness of these digital programmes over the next four years, however early results have shown that ‘the technologies could be cost effective’.
Currently, Liva can be used in the NHS, however the other three platforms recommended for use must first receive the relevant approval from NHS England.
According to the 2021 Health Survey for England, just over a quarter of adults were living with obesity and a further 37.9% were overweight.
NICE’s interim director of medical technology and digital evaluation Mark Chapman said: ‘Traditional face to face services treating people living with obesity are unable to keep up with demand. Waiting lists are long, some areas don’t have a service, and patients need a solution.
‘These four platforms could provide an option to accessing weight management support to those people who live in an area with no specialist weight management services or for those who are on a waiting list and are happy to be treated safely outside a hospital setting.’
Related Article: NICE recommends semaglutide for people with obesity
Health secretary Steve Barclay supported use of these apps, saying they will ‘improve access’ to support that helps tackle obesity.
He said: ‘The newest obesity medicines have the potential to help patients lose significant amounts of weight and reduce related conditions, but it’s vital they are used alongside diet, physical activity, and wider behavioural support to help stop people regaining weight.’
NICE cleared the use of diabetes drug semaglutide for obesity treatment in March this year although this usage is yet to be launched within the NHS.
Last week its manufacturer Novo Nordisk claimed that the drug can also reduce the risk of cardiovascular events by 20%.
However, there have been ongoing global shortages of semaglutide due to off-label prescribing, and last month GPs were advised to ‘discuss stopping’ its use for diabetes.
Related Article: Half of global population could be overweight by 2035, warns obesity charity
Leeds LMC recently warned that a lack of weight management services in the area, due to increased demand and lack of council funds, left patients with an ‘unacceptable’ service provision gap.
A version of this story first appeared on Pulse.

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom

