Encouraging Covid-19 vaccine uptake
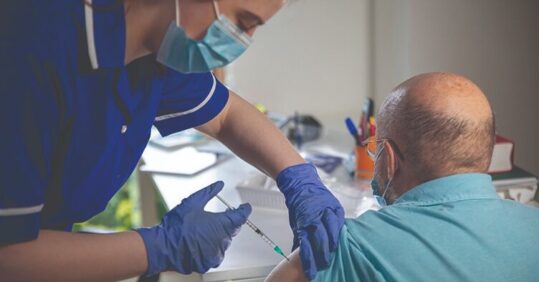
Elaine Francis, nurse clinical lead for Covid vaccination in North Tyneside, examines the ongoing challenges of vaccine hesitancy and continuing to promote uptake.
What are the ongoing challenges of vaccine hesitancy and continuing to promote uptake?
Working as clinical lead at three Covid vaccination sites has been a rollercoaster ride. People from every kind of background have come forward – eagerly or not-so-eagerly – to take part in the largest vaccination programme in history. The staggered initial rollout and the time scale of the vaccination schedule means that, after a huge spike in demand for boosters just before Christmas in response to Omicron, most people who were willing and able have now been fully vaccinated.
We’re now seeing more of those who had a reason to hold back. Some are women who avoided vaccination during pregnancy, having naturally been extra cautious; once pregnancy was included in the list of conditions with extreme vulnerability to complications from Covid there was an uptick in demand. However, there are still people who just don’t want the jab due to concerns over issues such as the apparent speed of the vaccines’ development, the potential for side-effects and whether ‘natural immunity’ is superior. Anecdotally, the main reason previously hesitant people finally came forward for their jab was the introduction of travel and employment restrictions – their desire to holiday or visit family abroad, or need to keep a job, outweighed their misgivings over the vaccine.
Related Article: Gypsy, Roma and Traveller healthcare: How can primary care serve this group?
The uptake of Covid vaccination across the UK has been impressive, with more than 90% of those aged 12 and over now having had at least their first dose. The aim, as with other routine immunisations, is for every eligible person to be vaccinated and although we now have the lifting of Covid restrictions across the UK, this remains important. The challenge now is to reach those who remain hesitant and that will require an approach that is honest, non-judgemental and non-confrontational, incorporating a thorough understanding of the rationale for vaccination and the skill to pitch the facts respectfully yet persuasively.
Is mandating vaccination wise?
The sense of being forced into something can be enough to make people mistrustful, polarise opinion and cause confrontation and resistance. Mandating what is, after all, a medical intervention can raise questions of informed consent, even bodily autonomy. The U-turn on mandatory vaccinations for NHS workers reflects some important aspects of public opinion, as well as the stark realities of a staffing crisis across the health service. We need to find better ways of promoting uptake than threatening people’s livelihoods.
A person-centred approach
Health promotion has always been a huge part of a practice nurse’s role, and this often means engaging with people who are unwilling to make choices that will improve their health and reduce their disease risk or the impact of existing conditions. Practice nurses are experienced in the kind of therapeutic interactions that balance people’s choices – including their freedom to make what we may consider unwise decisions – with informed health improvement.
Some of those who are resistant to having the vaccine will have legitimate questions. Others will be unable or unwilling to take in the full rationale for vaccination.
It’s important to remember that, as healthcare professionals, we are in the privileged position of having an inherent interest in and aptitude for evidence-based medicine. If we’re to encourage even a few of those people who have so far been reluctant to have the Covid vaccine, there must be room and capacity in our approach to address reasonable questions, but also to support those with different levels of understanding.
Related Article: Public urged to see practice nurse before travelling amid high enteric fever cases
Now that we’re vaccinating adolescents down to the age of 12, we’re even more likely to meet people who need to have information carefully pitched to their level of understanding. And as vaccinations for 5- to 11-year-olds roll out fully, we can expect an even wider range of responses, from the children themselves and from parents with their own ideas and fears about the safety implications of the vaccine in that age group.
Understanding opposition
Uncertainty about vaccines is nothing new; pamphlets from public dispensaries as far back as the very first smallpox inoculations in the 1780s reveal a familiar lament – people were worried about side-effects, more vocal about negative experiences than positive ones, and unable to afford to take time off work if they or their families became unwell. These are clearly basic needs and responses, and as the Covid vaccination programme becomes a regular aspect of our lives, we must build in an understanding of human behaviour and offer a practical, supportive response to misgivings.
The focus across the NHS is shifting from the huge logistical challenge of simply trying to make vaccines widely available to trying to understand why people might have been reluctant so far and to facilitate informed consent. Opinions are so polarised and views so entrenched at this stage that we need to create a culture where it’s okay to change your mind.1 We must allow that people will hear and read conflicting advice.
Crucially, people must feel they have the ultimate say in what happens to their bodies. What they need from us is tolerance, alongside evidence-based information about the benefits, for themselves and those around them, of vaccination, whether in the pandemic phase or going forward. We can help ensure they have the right knowledge to make their decisions.
Related Article: Current measles outbreaks could rise further this summer, UKHSA warns
Reference
- Integrated Covid Hub North East. Change of Heart Covid vaccination campaign. February 2022. Link

See how our symptom tool can help you make better sense of patient presentations
Click here to search a symptom




