Key learning points:
- Bronchiolitis is a clinical diagnosis and investigations are rarely indicated
- The majority of patients with bronchiolitis can be safely cared for at home
- No pharmacological treatments have been proven to be of benefit and treatment is largely supportive
Bronchiolitis is the most common lower respiratory tract infection in infants, affecting almost one-third of infants under the age of one.1 It is a seasonal illness with peak incidence in the winter months. Respiratory syncytial virus (RSV) is the cause in approximately 70% of cases.2
Although bronchiolitis remains the leading cause of hospitalisation of infants worldwide, the vast majority of those affected can be safely managed at home and in primary care, which bears the greatest burden of the disease.
Signs and symptoms
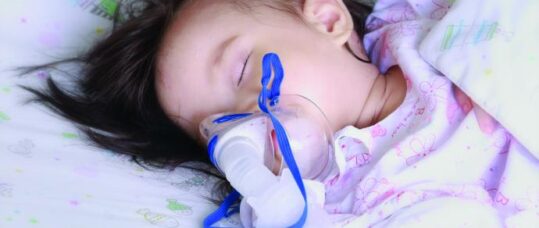
Parents often describe their children as initially being snuffly for one to two days, then they develop a persistent cough. They may experience difficulty breathing. A mild pyrexia and decreased feeding are also common. Some infants may vomit feeds.
Very young infants may present with apnoea as their only symptom. The illness peaks between days five to seven, although the cough may persist for weeks.
Risk factors for more severe disease include prematurity, chronic lung disease, immunodeficiency, airway defects, congenital heart disease and parental smoking. Breast feeding reduces the risk of bronchiolitis-related hospital admission.1,2,3
Diagnosis
Bronchiolitis is a clinical diagnosis and investigations are rarely indicated. The National Institute for Health and Care Excellence (NICE) recommends making a diagnosis based on the following clinical features:4
- Coryzal prodrome lasting one to three days.
- Persistent cough developing afterwards.
- Tachypnoea or chest recession.
- Wheeze or crackles on chest auscultation.
Assessment
Infants presenting to primary care should have a full set of checks including:
- Respiratory rate and an assessment of their work of breathing.
- Oxygen saturations (SpO2) with an appropriately sized probe.
- Temperature.
- Heart rate.
The Advanced Paediatric Life Support (APLS) Group outlines the normal values for respiratory rate and heart rate for various age groups.5
An assessment of hydration should also be performed, particularly if there has been a reduction in feed volumes to less than 50-75% of normal or there have been no wet nappies for 12 hours or longer.
Current best management
Traditionally nebulised therapies such as adrenaline, ipratropium bromide, salbutamol and hypertonic saline have been trialled in the management of bronchiolitis. Despite decades of research there is little evidence to suggest that any of these therapies lead to sustained and clinically significant improvements in outcomes.
The NICE guidelines therefore suggest that there are no pharmacological therapies that should be used routinely.4
Antibiotics are of no value in uncomplicated bronchiolitis as it is a viral illness. Consequentially treatment options in primary care are limited and the key decision is whether the infant is fit to be managed at home with advice or whether referral to hospital is required for supportive therapy such as oxygen, gentle nasopharyngeal suction and fluid support.
The NICE guidelines recommend immediate referral by emergency ambulance in cases where:
- Apnoea is observed or reported.
- The child looks seriously unwell to a healthcare professional.
- There is severe respiratory distress – grunting, marked recession or a respiratory rate of more than 70 breaths per minute.
- The child has central cyanosis.
- Sp02 is persistently below 92% when breathing air.
When deciding whether to refer, the guidelines also suggest that consideration should be given to the presence of any co-morbidities increasing the risk of severe disease and the social environment, including the parent’s ability to manage at home and recognise and respond to deteriorations. In infants who require an urgent transfer to hospital it would be appropriate to administer oxygen.
In those infants who are deemed fit to be managed at home, parents should be given the following advice:
1. Feeding: Offer small volumes of feeds more frequently. For infants who are not yet weaned, fluid requirement is usually 150ml/kg/day. While unwell with bronchiolitis an intake of approximately 75% or 110ml/kg/day would be acceptable.1,4
2. Handheld suction devices: These are increasingly available from community pharmacies. Parents often enquire about these devices. There is no evidence to support their use, but anecdotally parents have described benefit where secretions are hindering the infant’s ability to feed.
3. Infection control: Bronchiolitis is highly contagious. Transmission is both through aerosolised droplets and close contact with contaminated secretions. The virus can live for several hours on hard surfaces and 30 minutes on hands. The best way to reduce the spread of bronchiolitis is with regular hand-washing. Any toys that are shared among siblings should be disinfected regularly.6
4. Course of illness: It is useful to make parents aware of the natural course of bronchiolitis as described in the section on signs and symptoms. In particular, remind parents that the cough may persist for several weeks and that no treatment is needed for this in an otherwise well infant.
5. Antipyretics: Bronchiolitis is often associated with a mild pyrexia. Advise parents on appropriate dosing and use of paracetamol and/or ibuprofen. If the temperature is above 39°C it would be advised to attend for reassessment.4
6. Key safety information: NICE guidelines outline the following key safety information that should be provided to parents about caring for children at home:4
- How to recognise developing red flag symptoms, which includes worsening increased work of breathing, fluid intake less than 50-75% of normal or no wet nappy for 12 hours, apnoea and cyanosis. exhaustion.
- The importance of not smoking in the infant’s home.
- How to get help if required.
- Arrangements for follow-up if necessary.
In some areas, infants who have been hospitalised with bronchiolitis may be discharged on home oxygen in the recovery phase of their illness. Community nurses may be involved in facilitating this.
Palivizumab is a monoclonal antibody that may be administered (intramuscularly at monthly intervals) during the peak season for RSV bronchiolitis. Its use is restricted to high-risk infants, such as those with prematurity, chronic lung disease or congenital cardiac disease.
What the future holds
There is currently no routine vaccine available for bronchiolitis. Maternal immunisation is being evaluated for prevention of severe RSV disease in infants in the first six months of life.7
Bronchiolitis is a common illness in infancy and places a large burden on primary care services.
Treatment options for bronchiolitis are limited. The new NICE guidelines provide clear information on clinical features that
should encourage a positive diagnosis without need for further investigations. They also provide useful advice on which infants should be referred for further assessment and key safety information that should be given to parents for infants who are managed
at home.
References
1. McNaughten B, Bourke TW. Optimising the management of bronchiolitis in infants. Practitioner 2015;259:13-15
2. Bourke T, Shields M. Bronchiolitis. BMJ Clin Evid 2011;2011:0308
3. Budhiraja, S, Verma R, Shields M. The management of acute bronchiolitis in infants. Paediatr Child Health 2013;23:296-300
4. National Institute for Health and Care Excellence. NG9. Bronchiolitis in children. London: NICE;2015
5. Samuels M, Wieteska S, editors. Advanced Paediatric Life Support: A Practical Guide To Emergencies. 6th edition. Wiley Blackwell, 2016
6. Empey KM, Peebles RS, Kolls JK. Pharmacologic Advances in the Treatment and Prevention of Respiratory Syncytial Virus. Clinical infectious diseases: an official publication of the Infectious Diseases Society of America. 2010;50:1258-67
7. Munoz FM. Respiratory Syncytial Virus in Infants: Is Maternal Vaccination a Realistic Strategy? Curr Opin Infect Dis 2015;28:
221-4